Get the App
For Doctors
Login/Sign-up
About
Health Feed
Find Doctors
Health Packages
AllQ&AsTipsQuizzes
High Sugar Health Feed
Asked for female, 51 years old from Mumbai
Share
Bookmark
Report
Last Updated: 3 years ago• Featured Tip
Share
Bookmark
Report
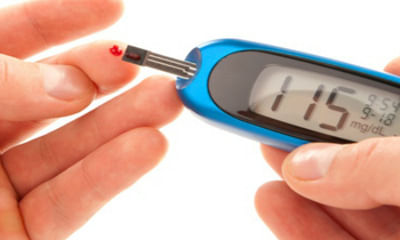
The other name of sugar level in the blood is Glycaemia. Sugar present in the blood is known as glucose. Glucose is the amount of sugar found in the blood. Sugar in the blood is the result of the amount of the food that we consume. It is the main source of energy. The blood is responsible for carrying the glucose to all the cells of the body.
If the sugar level in your blood increases, then it can lead to the disease known as diabetes. The symptoms of high levels of sugar in the blood a...more
If the sugar level in your blood increases, then it can lead to the disease known as diabetes. The symptoms of high levels of sugar in the blood a...more
Asked for female, 24 years old from Navi Mumbai
Share
Bookmark
Report
Health Query
Share
Bookmark
Report
These are symptoms of irritable bowl. Metformin may cause these symptoms. I would recommend to reduce dose of metformin to half of what you are taking. Do not take soda based drinks as it worsens irritable bowl. Try to reduce and gradually stop metformin by following strict diet and exercise. Also I would recommend you to check thyroid tests. Also try to avoid wheat/ maida completely for one month from your diet. This may help you. If still you find problems, please consult some other doctor.
695 people found this helpful
Asked for male, 62 years old from Pune
Share
Bookmark
Report
DHMS (Diploma in Homeopathic Medicine an...read more
Homeopathy Doctor•Hyderabad
You better have fasting blood sugar, post lunch blood sugar and hba1c tests to get accurate picture. *have vigorous physical exercise to improve absorption and blood circulation.*even with desk job, you can spend morning and evening time for work out
*take protein rich food --- seeds, pulses, nuts, also fruits, vegetables, greens and reduce cereals. *green tea is also good.
*avoid sweets, cakes, creams, fried foods, processed food and junk food. Avoid sugary soft drinks, sweetish juices.
*take protein rich food --- seeds, pulses, nuts, also fruits, vegetables, greens and reduce cereals. *green tea is also good.
*avoid sweets, cakes, creams, fried foods, processed food and junk food. Avoid sugary soft drinks, sweetish juices.
15 people found this helpful
Health Query
Share
Bookmark
Report
DHMS (Diploma in Homeopathic Medicine an...read more
Homeopathy Doctor•Hyderabad
You have high blood sugar. *take protein rich food --- seeds, pulses, nuts, also fruits, vegetables, greens and reduce cereals. *green tea is also good.
*avoid sweets, cakes, creams, fried foods, processed food and junk food. Avoid sugary soft drinks, sweetish juices
consult your endocrinologist as soon as possible.
*avoid sweets, cakes, creams, fried foods, processed food and junk food. Avoid sugary soft drinks, sweetish juices
consult your endocrinologist as soon as possible.
77 people found this helpful
Health Query
Share
Bookmark
Report
For this level you should consult a physicain or a diabetologist, who will have to conduct many other tests related to blood sugar and probable complications of diabetes. Initially insulin injections may also be required. May be temporarily. Otherwise you may land yourself in difficult situation. Treatment will be life long preferably under same doctor for follow up and review.
124 people found this helpful
Last Updated: 6 years ago• Featured Tip
Share
Bookmark
Report
Scientists have concluded that sugar stimulates the exact same centers of the brain which derive pleasure out of heroin or cocaine. For those who are addicted to sugar, getting off it leads to intense cravings and withdrawal symptoms. If you have an uncontrollable urge to devour something sweet, you probably have sugar addiction too. Sugar is known to release dopamine and opioids, which not only make it addictive but makes it extremely difficult for you to overcome the withdrawal symptoms.
...more
...more
Asked for female, 60 years old from Mumbai
Share
Bookmark
Report
Diabetologist•Marigaon
Last Updated: 6 years ago• Featured Tip
Share
Bookmark
Report
डायबिटीज के लिए ग्रीन टी: क्या ग्रीन टी ब्लड शुगर को कन्ट्रोल करने में मदद कर सकती है?
ग्रीन टी के कई स्वास्थ्य लाभ हैं जो बहुत से लोगों को नहीं पता हैं और उनमें से एक यह है कि ग्रीन टी मधुमेह (डायबिटीज) वाले लोगों के लिए भी अच्छी होती है।
ग्रीन टी पीना डायबिटीज से पीड़ित व्यक्तियों के लिए एक अच्छा विचार है क्योंकि यह ब्लड शुगर के स्तर को कम करने में मदद करता है। कई सकारात्मक परिणाम हैं कि अगर मधुमेह वाले लोग ग्रीन टी पीते हैं तो वे लंबे समय तक स्वस्थ रह सकते हैं।
डायब...more
ग्रीन टी के कई स्वास्थ्य लाभ हैं जो बहुत से लोगों को नहीं पता हैं और उनमें से एक यह है कि ग्रीन टी मधुमेह (डायबिटीज) वाले लोगों के लिए भी अच्छी होती है।
ग्रीन टी पीना डायबिटीज से पीड़ित व्यक्तियों के लिए एक अच्छा विचार है क्योंकि यह ब्लड शुगर के स्तर को कम करने में मदद करता है। कई सकारात्मक परिणाम हैं कि अगर मधुमेह वाले लोग ग्रीन टी पीते हैं तो वे लंबे समय तक स्वस्थ रह सकते हैं।
डायब...more
Book appointment with top doctors for High Sugar treatment
View fees, clinic timings and reviews
Ask a free question
Get FREE multiple opinions from Doctors
posted anonymously