Get the App
For Doctors
Login/Sign-up
About
Health Feed
Find Doctors
Health Packages
AllQ&AsTipsQuizzes
Skin Problems in Children Tips
Last Updated: 3 years ago• Featured Tip
Share
Bookmark
Report
General Physician•Alappuzha
;
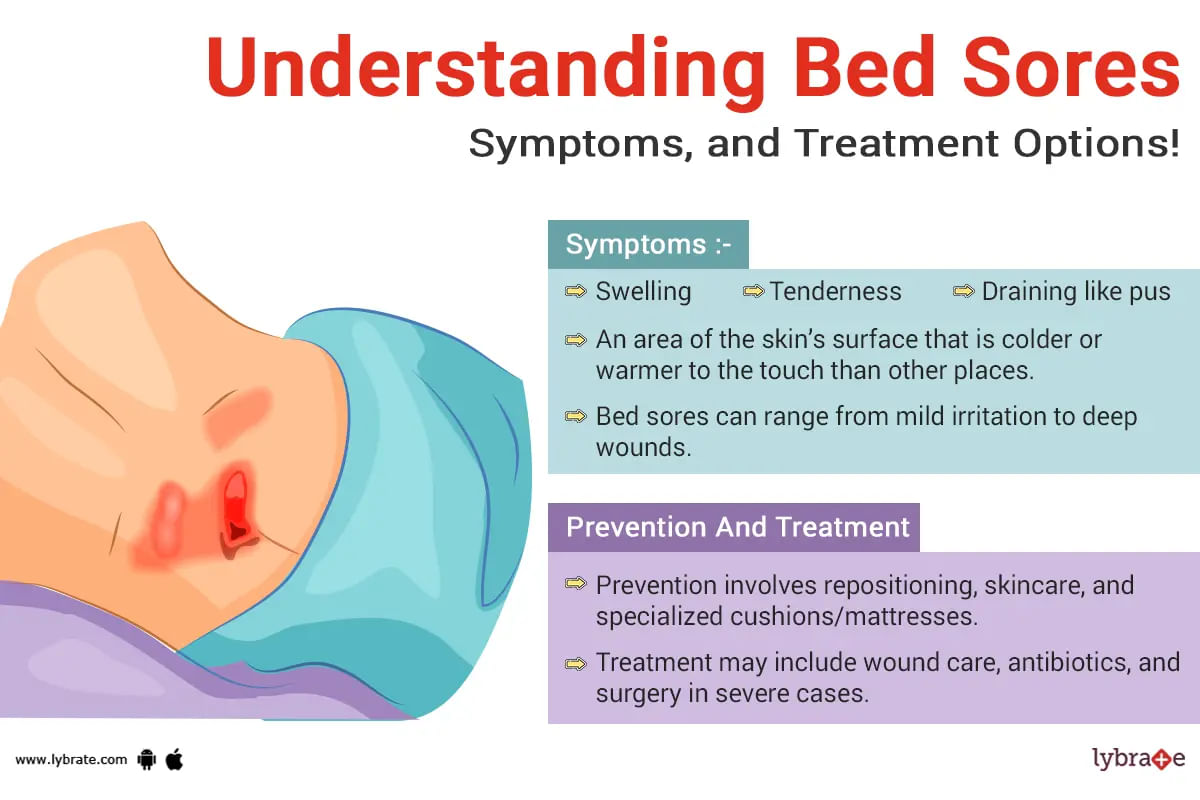
Bedsores: symptoms, causes and management
When we do some work for a long time or for the first time there is pressure on the skin of the area used for work, that pressure causes injury to skin and nearby tissue causing ulcers called pressure ulcers.
They are also known as bedsores and decubitus ulcers. Bedsores always happen to the place where skin is over bone and the gap between them is very low. Such areas are like heels, hands and sometimes...more
222 people found this helpful
Last Updated: 3 years ago• Featured Tip
Share
Bookmark
Report
General Physician•Sonipat
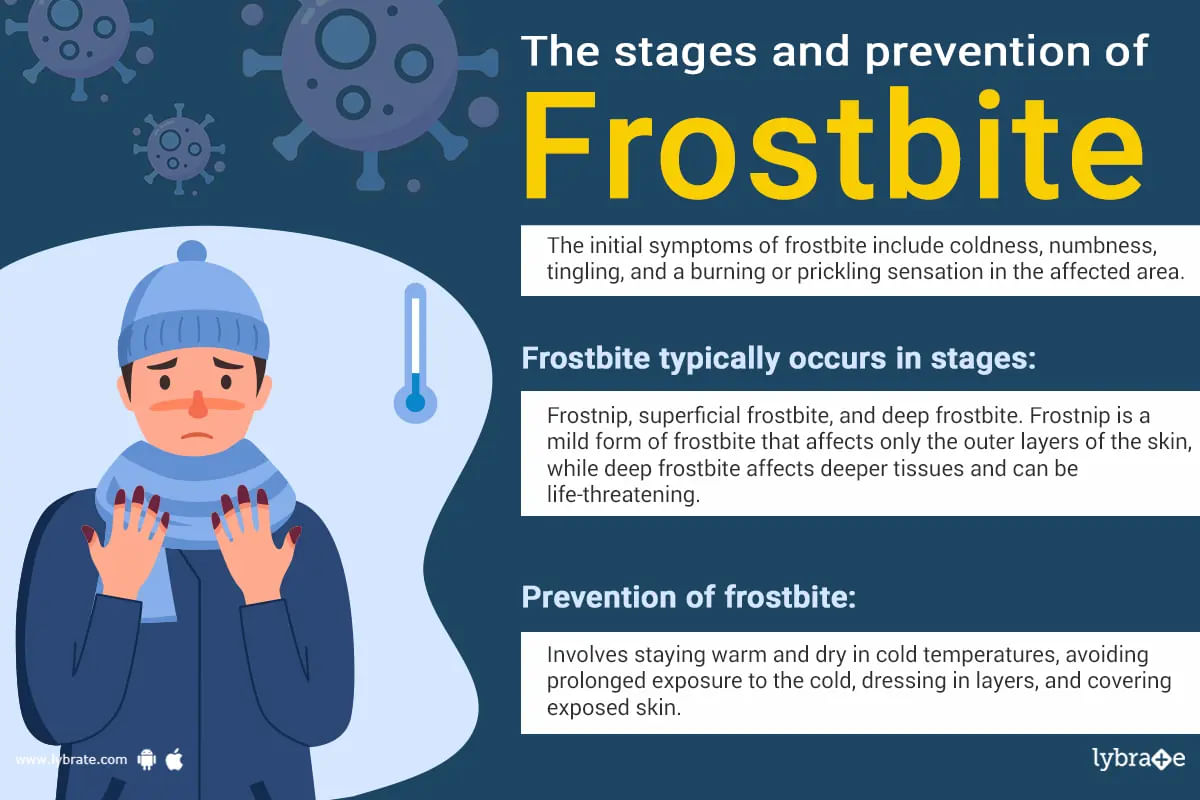
When there is freezing of skin due to the environment, there is injury, due to freezing, of the skin and the underlying tissues is called frostbite. There are stages of frostbite. Earliest stage is known as frostnip in which there is no permanent damage to tissue and layers of skin. ;
There are few symptoms like cold skin and itching feeling. After sometime symptoms are followed by numbness to inflammation and discoloration of skin. At late stage of frostbite the sym...more
Last Updated: 3 years ago• Featured Tip
Share
Bookmark
Report
1. Dr. Lipy gupta
Https://www. Lybrate. Com/delhi/doctor/dr-lipy-gupta-dermatologist-1
Md - dermatology, venereology & leprosy, mbbs
17 years experience 800 at clinic 1000 online
;
Dr. Lipy gupta is a distinguished dermatologist and member of the cosmetology society of india (cdsi). She was a former assistant professor at Dr. Ram manohar lohia hospital and pgimer. She has extensive experience treating a variety of skin ...more
Last Updated: 3 years ago• Featured Tip
Share
Bookmark
Report
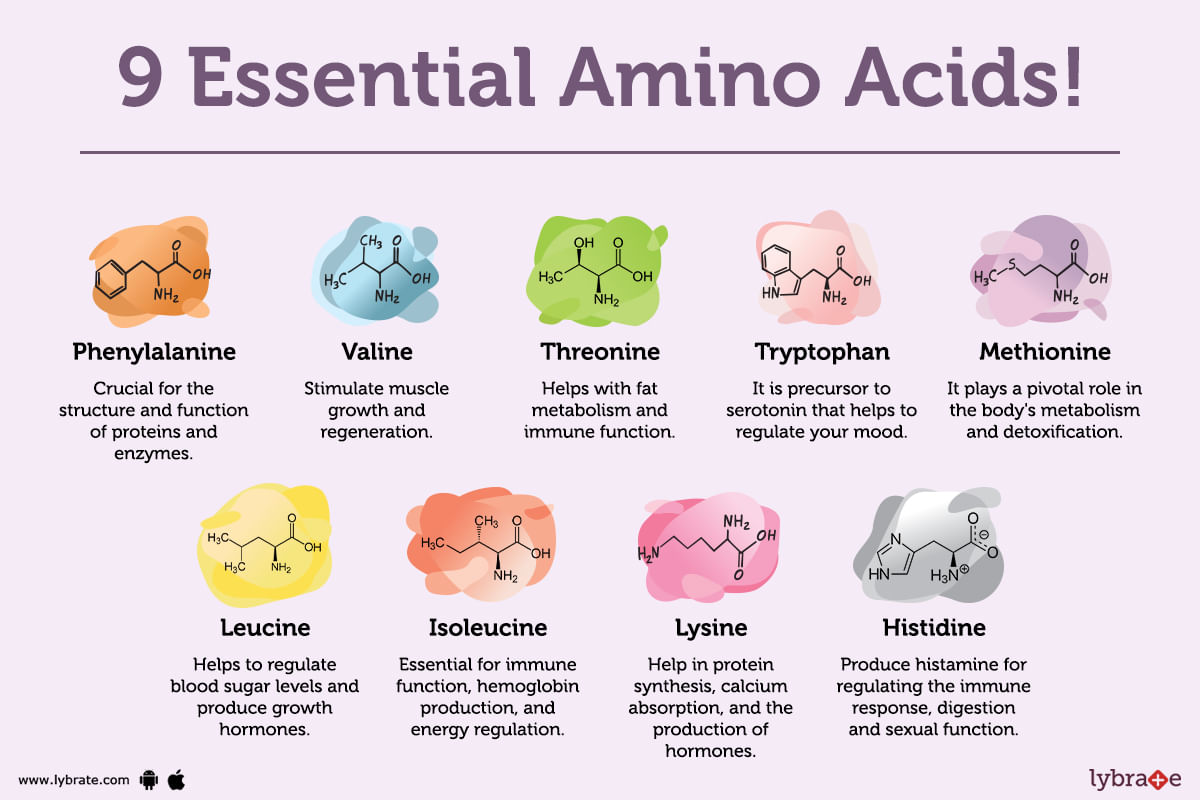
What are essential amino acids?
An essential amino acid can be best defined as an amino acid that the body cannot produce on its own, unlike nonessential amino acids. It must instead be obtained through food sources, diet, or supplementation.
Furthermore, it must be noted that out of the 20 amino acids your body needs for growth and function, as many as nine are considered essential. And as mentioned above, a human body is not capable of producing them on it...more
Last Updated: 3 years ago• Featured Tip
Share
Bookmark
Report
भारत में गोदना यानी कि टैटू का चलन आदिकाल से है। यहां तक कि पुराणों तक में इसका जिक्र मौजूद है। हालांकि पहले यह इतना प्रचलित नहीं था लेकिन बढ़ते समय के साथ ही अब युवाओं में इसका क्रेज बढ़ता ही जा रहा है। युवाओं में बढ़ते इस टैटू के क्रेज को ऐसे ही समझ सकते हैं कि कई युवा अपने शरीर पर एक या दो टैटू नहीं, बल्कि पूरे शरीर पर टैटू बनवाए नजर आ जाते हैं। तो चलिए जानते हैं कि टैटू के विषय में वो सारी बातें जिनका जानना आपके लिए बहुत जरूरी है। टैटू हमेशा एक प्रफेशनल आर्टिस्ट से ही बनवाना चाहिए, क्योंकि इसके...more
159 people found this helpful
Last Updated: 3 years ago• Featured Tip
Share
Bookmark
Report
1. Dr. Pradeep kumari
Https://www. Lybrate. Com/pune/doctor/dr-pradeep-kumari-dermatologist-1
Mbbs, md - dermatology, f. C. P. S.(dermatology, venereology & leprosy), dvd, dnb (dermatology)
20 years experience 700 at clinic
;
The dermatologist Dr. Pradeep kumari is very skilled and knowledgeable. Both the cosmetic dermatology society of india (cdsi) and the association of cosmetic surgeons of india hold her in high regard ...more
84 people found this helpful
Last Updated: 3 years ago• Featured Tip
Share
Bookmark
Report
Dermatologist•Kolkata
1. Dr. Anusree gangopadhyay
Https://www. Lybrate. Com/kolkata/doctor/dr-anusree-gangopadhyay-dermatologist
Mbbs, md - dermatology, specialty certificate, dermatology (uk)
14 years experience 600 - 990 at clinic
Dr. Anusree gangopadhyay is a renowned dermatologist who possesses a dermatology specialty certificate from the royal college of physicians and surgeons of the united kingdom. She earned a gold medal in medicine during her mbbs ...more
Last Updated: 3 years ago• Featured Tip
Share
Bookmark
Report
Many people are not born with perfect skin, and that's okay! our skin usually has a pigment called melanin, which gives it colour.
However, there are times when external factors such as heat, pollution, and bacteria can make our skin produce more melanin. This can cause our skin to tan. While some people may find tanned skin to be beautiful, others may want to know how to prevent their skin from getting darker.
If you are looking to lighten the skin tone and...more
Last Updated: 3 years ago• Featured Tip
Share
Bookmark
Report
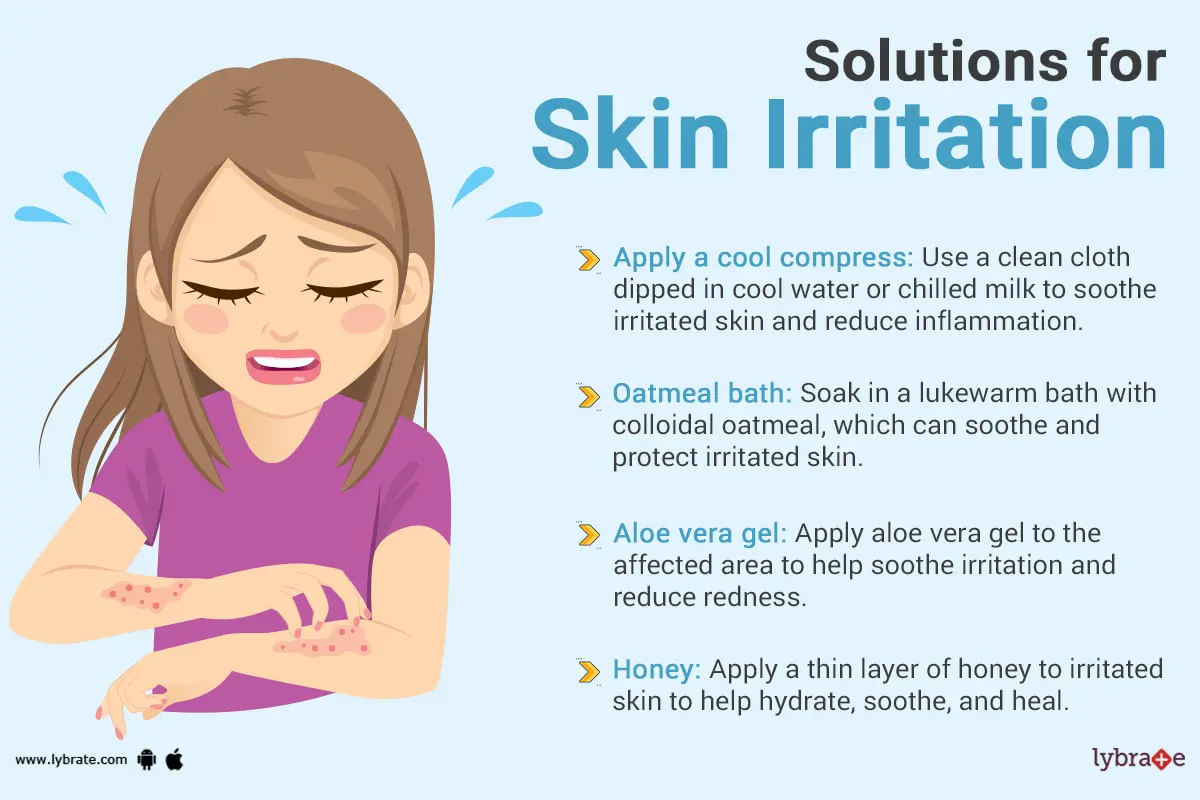
Skin irritation is a common problem faced by many in day to day life in the form of rashes, skin infections, itching etc. There are many irritants present in the environment which may cause these problems. Some of these irritants are pollen grains, waste products of animals, moulds etc. It is most commonly observed in the spring and summer season because of excessive sweating. Excessive sweating can trigger the symptoms of the allergic reactions. Some other products which may...more
Last Updated: 3 years ago• Featured Tip
Share
Bookmark
Report
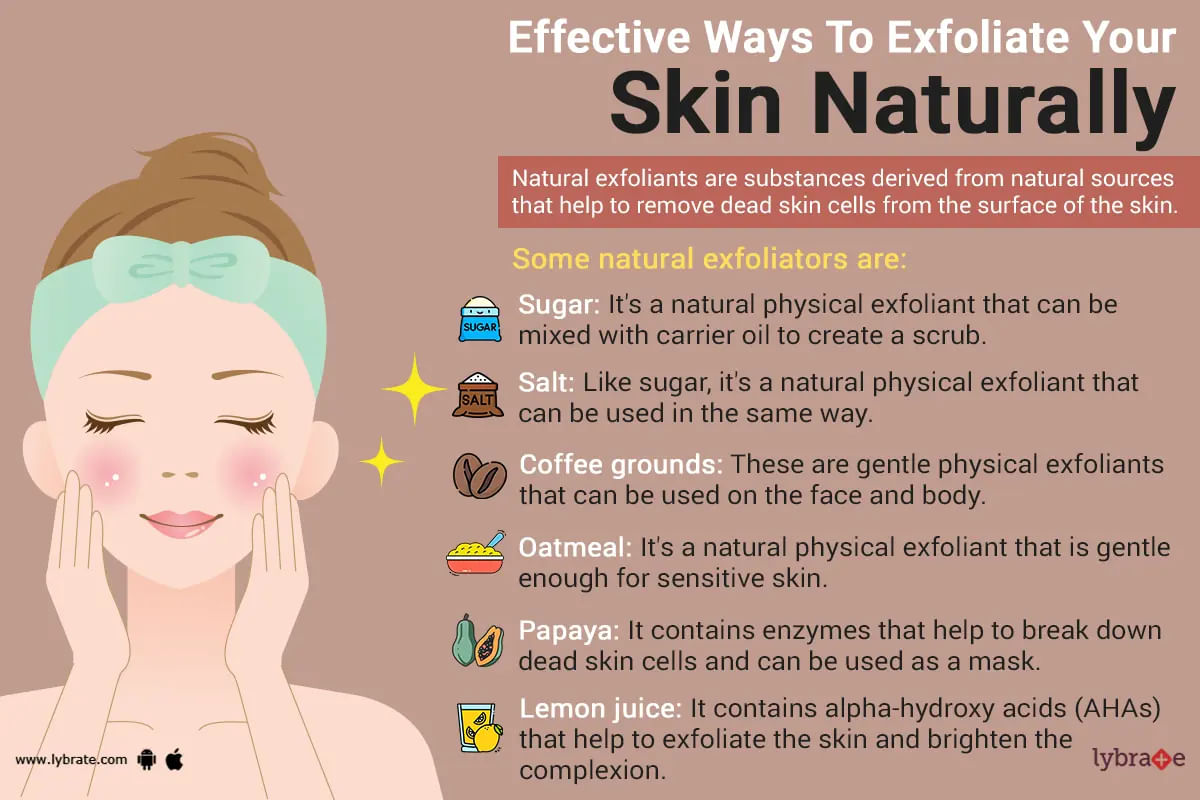
Exfoliation is the term given to the process of cleansing your skin with a product in order to achieve a smooth and clear complexion. Exfoliants, which are basically the products that a person applies to their skin, work by removing dead skin cells chemically or physically from the topmost layer of your skin.
Chemical exfoliants, which essentially contain alpha-hydroxy acids, come into action to break down or exfoliate dead skin on a molecular level. On the other han...more
Book appointment with top doctors for Skin Problems in Children treatment
View fees, clinic timings and reviews
Ask a free question
Get FREE multiple opinions from Doctors
posted anonymously