Get the App
For Doctors
Login/Sign-up
About
Health Feed
Find Doctors
Health Packages
AllQ&AsTipsQuizzes
Colon Cancer Tips
Last Updated: 5 years ago• Featured Tip
Share
Bookmark
Report
Minimal invasive surgery for rectal cancers has gained immense popularity and acceptance over open surgery in the last decade. Modern laparoscopic surgery is associated with minimal blood loss and pain with better short-term outcomes. The procedure ensures a speedy recovery and a decreased hospital stay. However, laparoscopic surgery has also been linked to high conversion rates (up to 29%) to open surgery, and those who were converted showed suboptimal outcomes.
To overcome the limita...more
To overcome the limita...more
Last Updated: 5 years ago• Featured Tip
Share
Bookmark
Report
A polyp is a cauliflower-like growth on the skin or the mucosal surface. Colon is the medical term for the larger intestine and the rectum. A growth on the mucosal surface of this part of the intestine is known as a colon polyp. Although not visible, colon polyps is present with symptoms, which can lead to their diagnosis. The main cause for concern is that some colon polyps can turn into colorectal cancer, which is the third largest cancer in America.
Types: There are two main types of...more
Types: There are two main types of...more
Last Updated: 5 years ago• Featured Tip
Share
Bookmark
Report
According to the American Cancer Society and Colon Cancer Alliance, colon cancer, which is also referred to as colorectal cancer is regarded as the third most commonly diagnosed type of cancer, as well as the second most important reason of cancer deaths in the U.S. affecting both men and women. But thankfully, colon cancer can be prevented by changing the food habits. It is also important to get regular screenings through colonoscopy, which will help you to determine the early or precancerous s...more
Last Updated: 6 years ago• Featured Tip
Share
Bookmark
Report
Cancer in colon forms due to uncontrolled cell growth in the large intestine cells. Most colon cancers originate from the healthy cells in the lining of the colon that grow into tumors called adenomatous polyps. These polyps can be cancerous or benign.
A cancerous tumor is malignant and may spread to the other parts of the body by traveling through blood and lymph systems, this process is known as metastasis. Whereas a benign tumor can grow but don t necessarily spread to other parts o...more
A cancerous tumor is malignant and may spread to the other parts of the body by traveling through blood and lymph systems, this process is known as metastasis. Whereas a benign tumor can grow but don t necessarily spread to other parts o...more
Last Updated: 6 years ago• Featured Tip
Share
Bookmark
Report
Diarrhea and constipation and common digestive ailments but if these persist for over 4 weeks, it could be a sign of colon cancer. Colon cancer refers, to a type of cancer that affects the lower half of the digestive system and the large intestines. In most cases, this type of cancer begins in the form of small adenomatous polyps. However, with time, these polyps turn cancerous.
As mentioned above a change in bowel movements is one of the main signs of colon cancer. Some of the other co...more
As mentioned above a change in bowel movements is one of the main signs of colon cancer. Some of the other co...more
Last Updated: 6 years ago• Featured Tip
Share
Bookmark
Report
MCh - Surgical Gastroenterology/G.I. Sur...read more
Surgical Gastroenterologist•Delhi
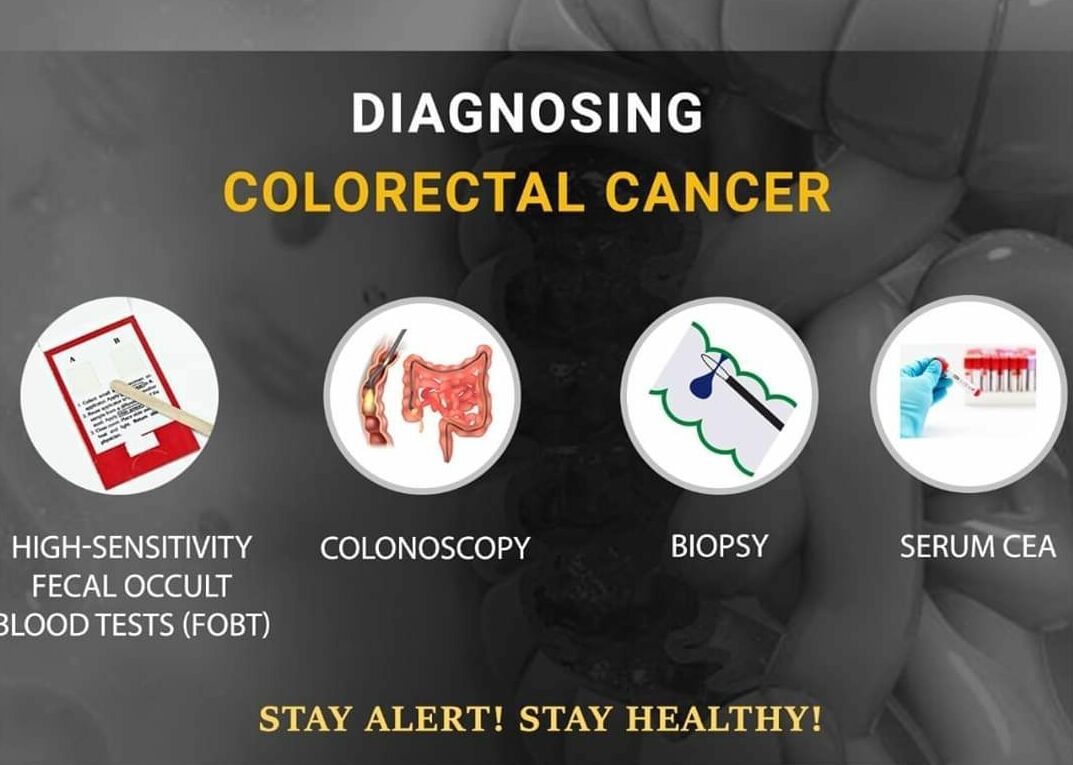
If someone has symptoms and signs of colon or rectal cancer, the doctor will suggest these tests for making the diagnosis.
Faecal immunochemical test for occult blood: this test is done on stool. It is used mostly as a screening test.
Colonoscopy: it is a procedure in which a flexible thin tube with a camera is passed and colon is seen from inside.
Biopsy: if any abnormality is seen on colonoscopy then a tiny bit of it is taken and examined under a microscope.
Serum CEA: CEA...more
Faecal immunochemical test for occult blood: this test is done on stool. It is used mostly as a screening test.
Colonoscopy: it is a procedure in which a flexible thin tube with a camera is passed and colon is seen from inside.
Biopsy: if any abnormality is seen on colonoscopy then a tiny bit of it is taken and examined under a microscope.
Serum CEA: CEA...more
Last Updated: 6 years ago• Featured Tip
Share
Bookmark
Report
Rectal cancer is the growth of cancerous cells in the rectum, which is the colon s lower part of the colon, connecting the large bowel and the anus. The basic function of the rectum is to collect the stool that is formed inside the human body before it is eliminated from the body. Cancer starts as a polyp, which is precancerous, and slowly develops and turns cancerous. This cancer will start spreading and penetrates into the walls of the rectum causing rectal cancer.
Surgery is the most...more
Surgery is the most...more
Last Updated: 6 years ago• Featured Tip
Share
Bookmark
Report
Cancer, in any form, is a deadly disease that requires immediate attention and treatment. Colon cancer is a common form of the disease, with over 10 lakh people reportedly affected in India each year.
In some cases, surgery is the only remedy for colon cancer. Depending on the progression of your cancer, if surgery becomes necessary, you should consider undergoing laparoscopic surgeries.
What is a laparoscopic surgery?
While most surgeries are open, where a large incis...more
In some cases, surgery is the only remedy for colon cancer. Depending on the progression of your cancer, if surgery becomes necessary, you should consider undergoing laparoscopic surgeries.
What is a laparoscopic surgery?
While most surgeries are open, where a large incis...more
Last Updated: 6 years ago• Featured Tip
Share
Bookmark
Report
Colon cancer is believed to be one of the common types of cancer affecting people. As the name suggests, here, the point of origin of the cancer is the colon or the large intestine. Though colon cancer can affect anyone, people with unhealthy lifestyle (sedentary) and habits (excess smoking and consumption of alcohol), obesity, certain medical conditions like diabetes, or exposed to radiations (radiation therapy) are at a greater risk of colon cancer. Colon cancer may also be hereditary.
more
Last Updated: 6 years ago• Featured Tip
Share
Bookmark
Report
Constipation refers to infrequent, painful bowel movements that are hard to pass. It is a common digestive issue, affecting about 22% of Indians. Although constipation is likely to affect all age groups, elderly people above age 65 suffer the most.
A person is said to have constipation under the following conditions
Fewer than three bowel movements in a week
Trouble passing stools
Having dry, hard, unusually large stools The reasons why people get ...more
A person is said to have constipation under the following conditions
Fewer than three bowel movements in a week
Trouble passing stools
Having dry, hard, unusually large stools The reasons why people get ...more
Book appointment with top doctors for Colon Cancer treatment
View fees, clinic timings and reviews
Ask a free question
Get FREE multiple opinions from Doctors
posted anonymously