Get the App
For Doctors
Login/Sign-up
About
Health Feed
Find Doctors
Health Packages
AllQ&AsTipsQuizzes
Ulcer Tips
Last Updated: 6 years ago• Featured Tip
Share
Bookmark
Report
Peptic Ulcers are sores that develop in the lining of a stomach, small intestine or lower oesophagus. They usually crop as a result of inflammation caused by bacteria and also due to erosion from stomach acids. Peptic Ulcers affecting the stomach are also known as gastric ulcer, one in the duodenum is called a duodenal ulcer and an ulcer occurring in the oesophagus is called an oesophageal cancer.
Talking about the causes, symptoms, tests and exams related to it and treatment options f...more
Talking about the causes, symptoms, tests and exams related to it and treatment options f...more
Last Updated: 6 years ago• Featured Tip
Share
Bookmark
Report
Peptic ulcers are wounds that develop in the stomach lining, less esophagus or small intestine. They are usually due to inflammation caused by bacterial H. pylori, in addition to corrosions from stomach acids. An ulcer is generally rooted in the stomach or inner layer of the small intestine. A stomach ulcer is the most visible sign of peptic an ulcer disease.
People with an ulcer may have a really hard time dealing with it. It is an open wound on the outer or internal surface of the bod...more
People with an ulcer may have a really hard time dealing with it. It is an open wound on the outer or internal surface of the bod...more
Last Updated: 6 years ago• Featured Tip
Share
Bookmark
Report
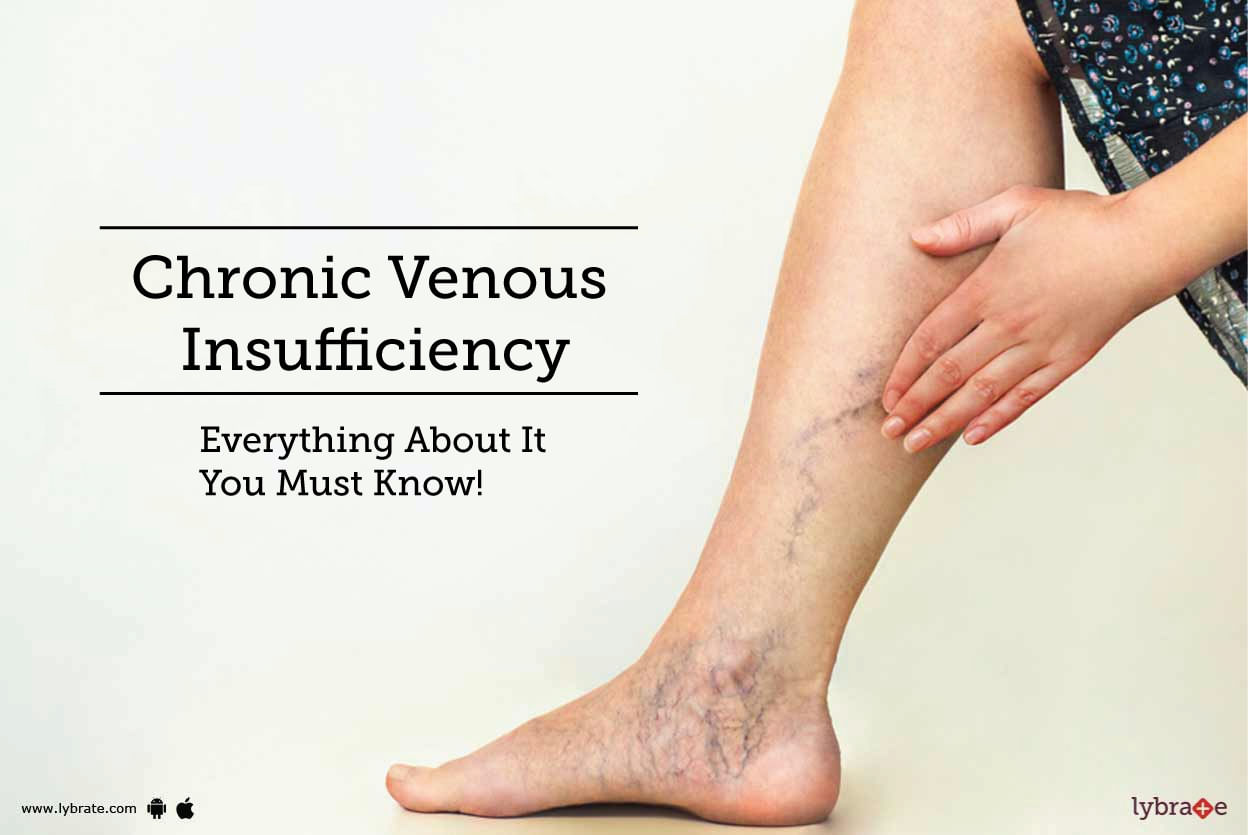
Chronic Venous Insufficiency is an abnormal condition of the leg veins. It occurs when either the walls or the one-way valves of the veins cannot work effectively. This
makes it difficult for the veins to send the impure blood from the legs to the heart. This results in impure flowing backward and collecting at places in the veins. It can
cause swelling, pain, and changes in skin and over time may lead to ulcers in legs.
Causes of Chronic Venous Insufficiency
Veins retu...more
makes it difficult for the veins to send the impure blood from the legs to the heart. This results in impure flowing backward and collecting at places in the veins. It can
cause swelling, pain, and changes in skin and over time may lead to ulcers in legs.
Causes of Chronic Venous Insufficiency
Veins retu...more
Last Updated: 6 years ago• Featured Tip
Share
Bookmark
Report
What is a peptic ulcer?
Digestive juices help in digestion of food but when these digestive juices damage the membrane of the digestive tract then sore areas develop which are called as peptic ulcers. A peptic ulcer may develop inlining of the lower oesophagus, stomach or duodenum. Thus called oesophageal, gastric and duodenal ulcer respectively.
Risk factors
NSAIDs- repeated use of NSAIDs irritate the wall of the stomach thus increase the acid secretion.
Stress al...more
Digestive juices help in digestion of food but when these digestive juices damage the membrane of the digestive tract then sore areas develop which are called as peptic ulcers. A peptic ulcer may develop inlining of the lower oesophagus, stomach or duodenum. Thus called oesophageal, gastric and duodenal ulcer respectively.
Risk factors
NSAIDs- repeated use of NSAIDs irritate the wall of the stomach thus increase the acid secretion.
Stress al...more
Last Updated: 6 years ago• Featured Tip
Share
Bookmark
Report
Ulcer pain can be uneasy and unbearable at times. It is caused by a bacterium known as the H. Pylori. Pain medication, lifestyle changes, and healthy eating habits can ensure pain relief from this condition. Here is a list of 4 best ways to get instant pain relief from an ulcer:
Medication - H. Pylori is often found in the digestive tract. Doctors suggest various combinations of antibiotics kill this bacterium. Some of those include tetracycline, levofloxacin, metronidazole, and tinidaz...more
Medication - H. Pylori is often found in the digestive tract. Doctors suggest various combinations of antibiotics kill this bacterium. Some of those include tetracycline, levofloxacin, metronidazole, and tinidaz...more
Last Updated: 6 years ago• Featured Tip
Share
Bookmark
Report
What are oral ulcers?
Canker sores or mouth ulcers are usually small, round or oval shaped, painful, red ulcers in the oral cavity on the mucous membrane.
Location may be inside of cheeks, floor of mouth, gums or tongue. The ulcers usually start appearing in childhood and resolve by thirties.
Types of mouth ulcers:
Minor ulcers are 2-7mm in diameter and usually resolve early within a fortnight.
Major ulcers are big, deep ulcers with irregular edged with punched out ...more
Canker sores or mouth ulcers are usually small, round or oval shaped, painful, red ulcers in the oral cavity on the mucous membrane.
Location may be inside of cheeks, floor of mouth, gums or tongue. The ulcers usually start appearing in childhood and resolve by thirties.
Types of mouth ulcers:
Minor ulcers are 2-7mm in diameter and usually resolve early within a fortnight.
Major ulcers are big, deep ulcers with irregular edged with punched out ...more
Last Updated: 6 years ago• Featured Tip
Share
Bookmark
Report
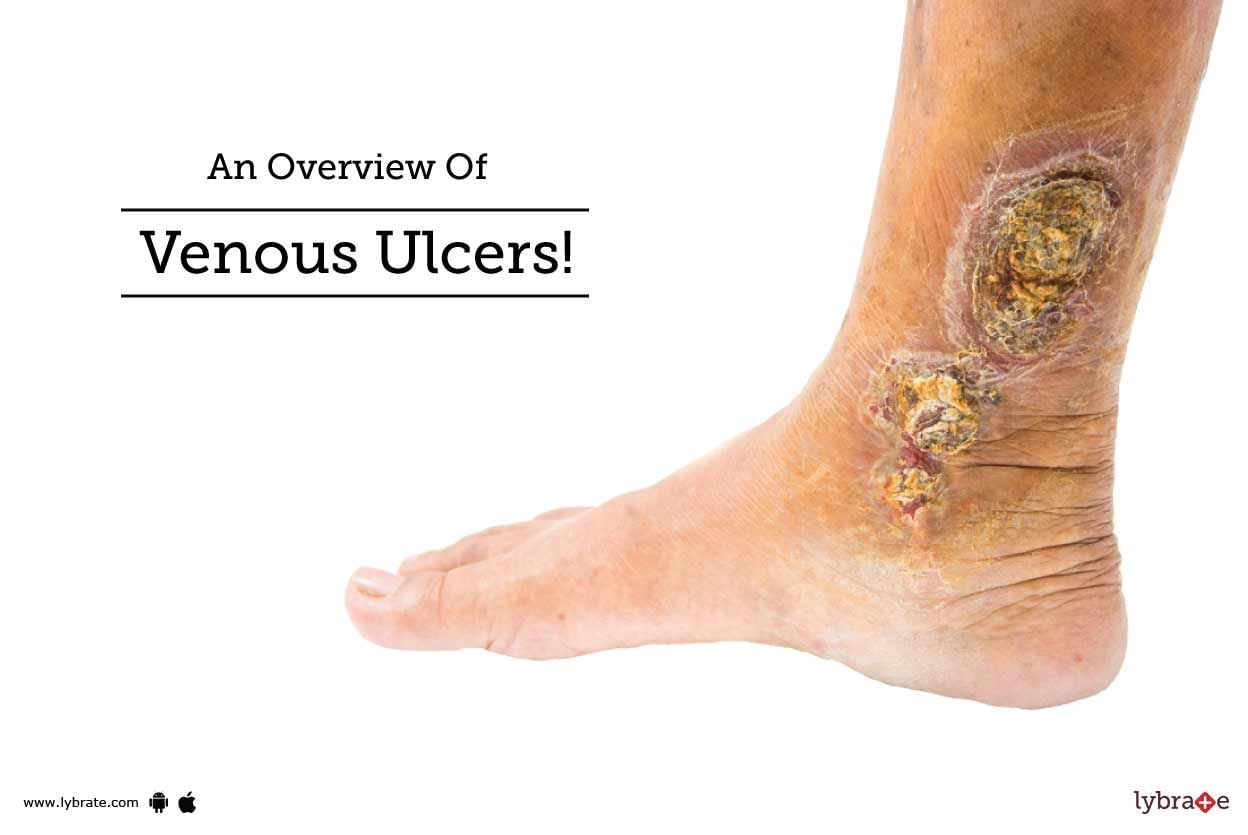
Venous Ulcers are also known as venous skin ulcers. They are nothing but slow-healing sores on legs that primarily result from weak blood circulation to the limbs. Such ulcers may last a few weeks or even years. However, one needs to get them treated since it may worsen the problem.
What Causes Venous Ulcers?
It may happen if there is a break in the skin around one of the ankles. The leg veins, which send impure blood to the heart may become weak and not work well enough. In most ca...more
What Causes Venous Ulcers?
It may happen if there is a break in the skin around one of the ankles. The leg veins, which send impure blood to the heart may become weak and not work well enough. In most ca...more
Last Updated: 6 years ago• Featured Tip
Share
Bookmark
Report
Many times we forget about the importance of our health in the race to pursue our careers and goals. We take our bodies for granted and keep working them without stopping for a breath. While some may have mastered this art, there are many who may not be able to cope with such a lifestyle and may end up falling ill. The most common problem that most people suffer from is stomach upset, gas, or stomach pain, and all of this may be because of not eating right or having irregular eating habits.
...more
...more
Last Updated: 6 years ago• Featured Tip
Share
Bookmark
Report
Ulcerative colitis is a chronic inflammatory condition whereby tiny abscesses and ulcers are formed on the inner lining of the large intestine, or on the colon or rectum. These ulcers may burst frequently resulting in diarrhea and bloody stools. This disease may also be responsible for causing anemia as well as harsh abdominal pain.
Ulcerative colitis normally alternates periodically from flaring up to receding quickly. These periods of remission can either last for weeks or maybe, even for ...more
Ulcerative colitis normally alternates periodically from flaring up to receding quickly. These periods of remission can either last for weeks or maybe, even for ...more
Last Updated: 6 years ago• Featured Tip
Share
Bookmark
Report
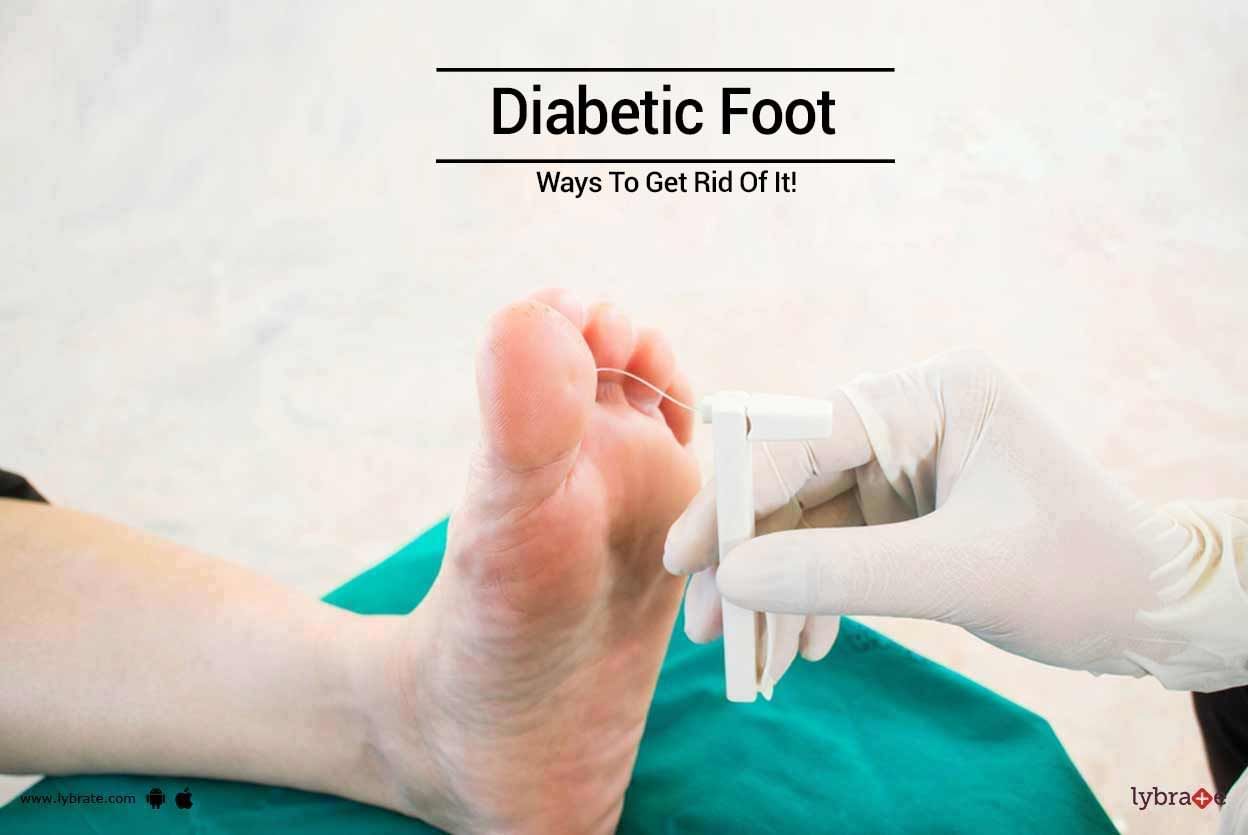
People who suffer from diabetes follow a strict diet and engage in strenuous exercises to stay healthy. However, most people tend to neglect a serious problem that may arise from diabetes. A condition known as diabetes foot may afflict your feet if proper care is not taken once diabetes is diagnosed. In fact, in severe cases, amputation may be the only way to treat diabetes foot.
How you can prevent diabetes foot
Here are some of the preventive measures you should adopt if you are s...more
How you can prevent diabetes foot
Here are some of the preventive measures you should adopt if you are s...more
Book appointment with top doctors for Ulcer treatment
View fees, clinic timings and reviews
Ask a free question
Get FREE multiple opinions from Doctors
posted anonymously