Get the App
For Doctors
Login/Sign-up
Health Feed
Find Doctors
Health Packages
AllQ&AsTipsQuizzes
Sports Fracture Rehabilitation Tips
Last Updated: 3 years ago• Featured Tip
Share
Bookmark
Report
1. Dr. Jitender pal singh
Https://www. Lybrate. Com/delhi/doctor/dr-jitender-pal-singh-orthopedist
Mbbs, Ms. - (orthopedics)
12 years of experience, rs. 600 in clinic, rs. 400 online
Dr. Jitendra pal singh is a renowned orthopedist who treats patients suffering from chronic pain, injuries to the hip, ankle, and knee, as well as a number of other disorders. At the moment, he is employed at the bone and joint clinic, which is located in the punjabi bagh neighbou...more
Https://www. Lybrate. Com/delhi/doctor/dr-jitender-pal-singh-orthopedist
Mbbs, Ms. - (orthopedics)
12 years of experience, rs. 600 in clinic, rs. 400 online
Dr. Jitendra pal singh is a renowned orthopedist who treats patients suffering from chronic pain, injuries to the hip, ankle, and knee, as well as a number of other disorders. At the moment, he is employed at the bone and joint clinic, which is located in the punjabi bagh neighbou...more
Last Updated: 3 years ago• Featured Tip
Share
Bookmark
Report
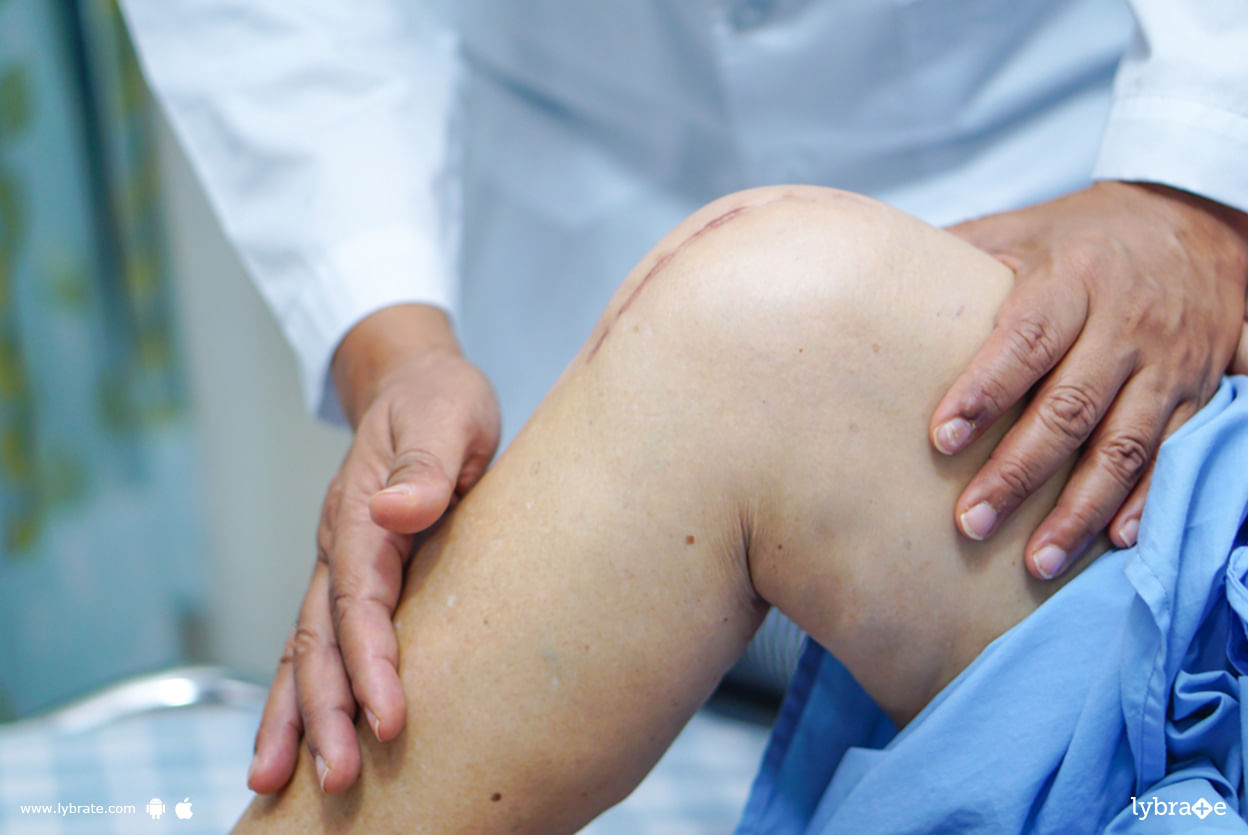
घुटना हमारे शरीर के सबसे महत्वपूर्ण जोड़ों में से एक है।इसमें तीन मुख्य हड्डियां जुड़ती हैं: फीमर, या जांघ की हड्डी; टिबिया, या पिंडली की हड्डी; और पटेला, या घुटने की कटोरी।एंटीरियर क्रूसिएट लिगामेंट (एसीएल) घुटने के केंद्र में होता है और पैर के रोटेशन और टिबिया के आगे की गति को सीमित करता है। एसीएल अक्सर अचानक पैर के मुड़ने से घायल हो जाता है। आप जिस दिशा में जा रहे हैं अगर तुरंत उसे बदलकर दूसरी दिशा में घूम जाते है तो आप अपने एसीएल को घायल कर सकते हैं। दौड़ते समय अचानक रुक ...more
Last Updated: 5 years ago• Featured Tip
Share
Bookmark
Report
MBBS Bachelor of Medicine and Bachelor o...read more
Orthopedic Doctor•Bhubaneswar
The anterior cruciate ligament (acl) is a rope like connective tissue that gives support and stability to the knee, along with other related tissues. If you do not repair it, you can still perform many functions, and carry on with your life with little difficulty. However, surgery to correct the ligament tear is recommended if you do not want the injury to impede your sporting activities and want a 100% normal knee.
The acl reconstruction surgery can be performed in two ways, the arthro...more
The acl reconstruction surgery can be performed in two ways, the arthro...more
Last Updated: 5 years ago• Featured Tip
Share
Bookmark
Report
MBBS Bachelor of Medicine and Bachelor o...read more
Orthopedic Doctor•Bhubaneswar
One of the most common injuries in sports is a stress fracture. Overcoming an injury like a stress fracture can be difficult, but it can be done.
A stress fracture is an overuse injury. It occurs when muscles become fatigued and are unable to absorb added shock. Eventually, the fatigued muscle transfers the overload of stress to the bone causing a tiny crack called a stress fracture.
Causes :
Stress fractures often are the result of increasing the amount or intensity o...more
A stress fracture is an overuse injury. It occurs when muscles become fatigued and are unable to absorb added shock. Eventually, the fatigued muscle transfers the overload of stress to the bone causing a tiny crack called a stress fracture.
Causes :
Stress fractures often are the result of increasing the amount or intensity o...more
Last Updated: 5 years ago• Featured Tip
Share
Bookmark
Report
MBBS, MS - Orthopedics, Fellowship, Depu...read more
Orthopedic Doctor•Bhubaneswar
Rotator Cuff Tear is one of the most common disabilities observed amongst adults above 40 years of age. Rotator Cuff is a group of four muscles that keep the Humerus (arm bone) attached to the socket of the Shoulder. The Rotator Cuff keeps the Shoulder Blade attached to the arm, and when there s damage (tear) in one of these muscles, excruciating pain is felt by the patient.
Kinds of Rotator Cuff Tear-
Partial Tear: This happens when one of the Tendons amongst the four Tendon...more
Kinds of Rotator Cuff Tear-
Partial Tear: This happens when one of the Tendons amongst the four Tendon...more
Last Updated: 5 years ago• Featured Tip
Share
Bookmark
Report
The spinal cord is such a crucial part of the body, and an injury to it can really change people s lives for the worse. After all, controlling our movements, our sense of feeling and directing the limbs, among other things, makes it so very important. It does happen sometimes that injury to it requires surgery. Isn t the prospect of the surgery going wrong quite a scary one?
For decades, whenever surgery to the spine was required, the surgeon needed to cut open the skin covering the spi...more
For decades, whenever surgery to the spine was required, the surgeon needed to cut open the skin covering the spi...more
Last Updated: 6 years ago• Featured Tip
Share
Bookmark
Report
Medial Patellofemoral Ligament (MPFL) helps in stabilizing the knee. It also prevents the knee from dislocating or moving outward. It is responsible to attach the patella (kneecap) to the femur (thigh bone). Together, these bones form the patellofemoral joint.
The dislocation of the patella or kneecap is the most common reason for the MPFL to get injured. Individuals with weak leg muscles, ligament laxity, deformed knee, etc., are at a greater risk of patella dislocation. Sportsperson ...more
The dislocation of the patella or kneecap is the most common reason for the MPFL to get injured. Individuals with weak leg muscles, ligament laxity, deformed knee, etc., are at a greater risk of patella dislocation. Sportsperson ...more
Last Updated: 6 years ago• Featured Tip
Share
Bookmark
Report
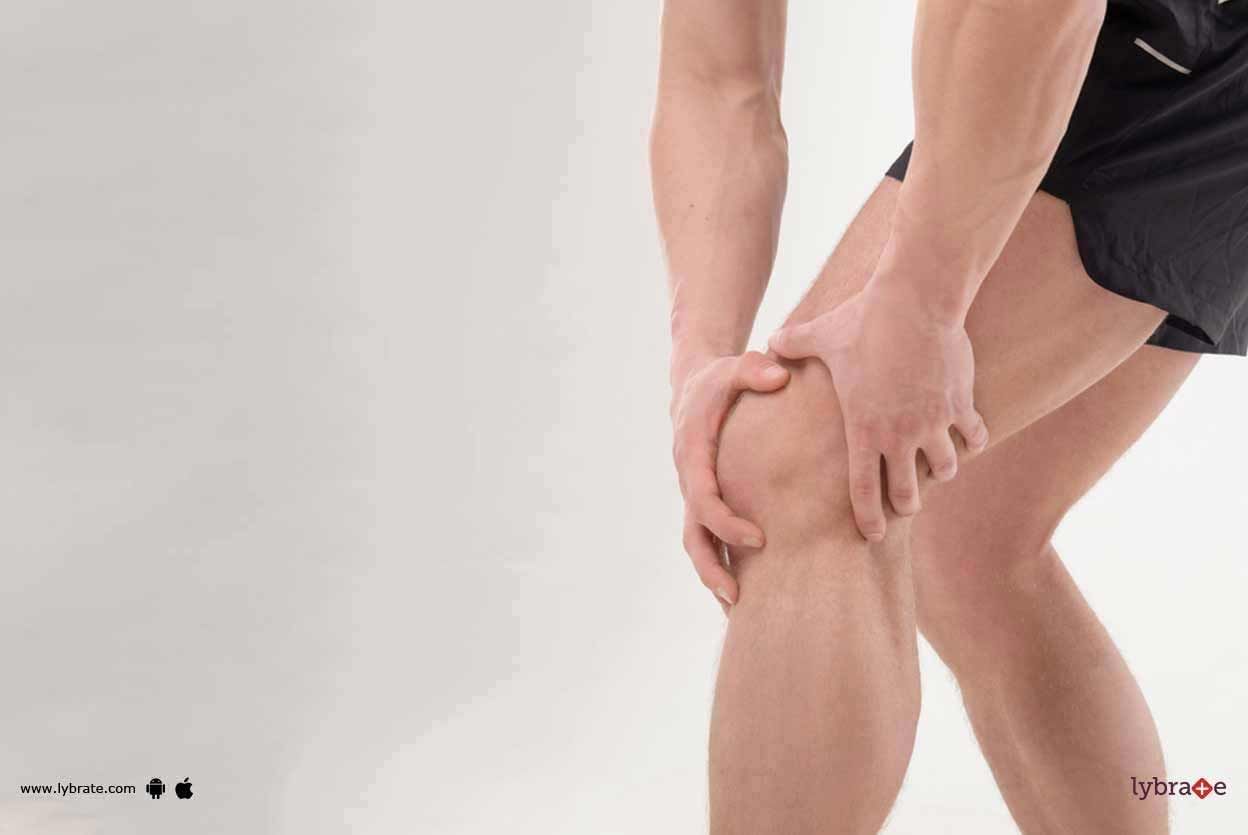
Too much of something is never a good idea. Running is a great way to exercise, but if you don't run in moderation and do not take care of yourself, you could foresee more than one health problem. If you push yourself too hard as a runner, you could face one or more of these running problems.
Runner's knee: If the bones in your knee shift out of alignment, the condition is called runner's knee. This is one of the most common overuse injuries. At first, you may not realize it, but with t...more
Runner's knee: If the bones in your knee shift out of alignment, the condition is called runner's knee. This is one of the most common overuse injuries. At first, you may not realize it, but with t...more
Last Updated: 6 years ago• Featured Tip
Share
Bookmark
Report
Knee problems can be quite annoying but if this problem becomes regular, it brings life to a standstill. The movement becomes restricted. Many associated problems slowly crop up. Thus, it is best to nip the problem in the bud. While some people might experience a problem in the full knee, in some people, only a single compartment (tissue or cartilage) of the knee may be affected. For such patients, Unicondylar Knee Replacement comes as a blessing.
The Unicondylar knee replacement, also ...more
The Unicondylar knee replacement, also ...more
Last Updated: 6 years ago• Featured Tip
Share
Bookmark
Report
What is Articular Cartilage Injury?
Cartilage is an important structural unit of the body. It is present in places like the joints, the spine, the end of ribs, in the bronchial tubes, and the ear and the nose. Cartilages are firm, but flexible tissues. There are many types of cartilages found in the body. Among them, articular cartilages are the ones that are present on the surface of the bones. As the name suggests articular cartilages exist to render articulation to the bones and retain t...more
Cartilage is an important structural unit of the body. It is present in places like the joints, the spine, the end of ribs, in the bronchial tubes, and the ear and the nose. Cartilages are firm, but flexible tissues. There are many types of cartilages found in the body. Among them, articular cartilages are the ones that are present on the surface of the bones. As the name suggests articular cartilages exist to render articulation to the bones and retain t...more
Book appointment with top doctors for Sports Fracture Rehabilitation treatment
View fees, clinic timings and reviews
Ask a free question
Get FREE multiple opinions from Doctors
posted anonymously