Get the App
For Doctors
Login/Sign-up
About
Health Feed
Find Doctors
Health Packages
AllQ&AsTipsQuizzes
Skin Scars Tips
Last Updated: 6 years ago• Featured Tip
Share
Bookmark
Report
Dermabrasion is a cosmetic procedure to resurface the uppermost layer of the skin which contains dirt and dead cells. This cosmetic procedure is suggested to the patients with fine lines, patches, scars, or pores. The procedure is done by using a rolling device which is rolled on the skin and the dirt or dead layer is removed.
While undergoing the dermabrasion procedure, the doctors will numb your skin area. You can also be given general anaesthesia depending upon the length and complic...more
While undergoing the dermabrasion procedure, the doctors will numb your skin area. You can also be given general anaesthesia depending upon the length and complic...more
Last Updated: 6 years ago• Featured Tip
Share
Bookmark
Report
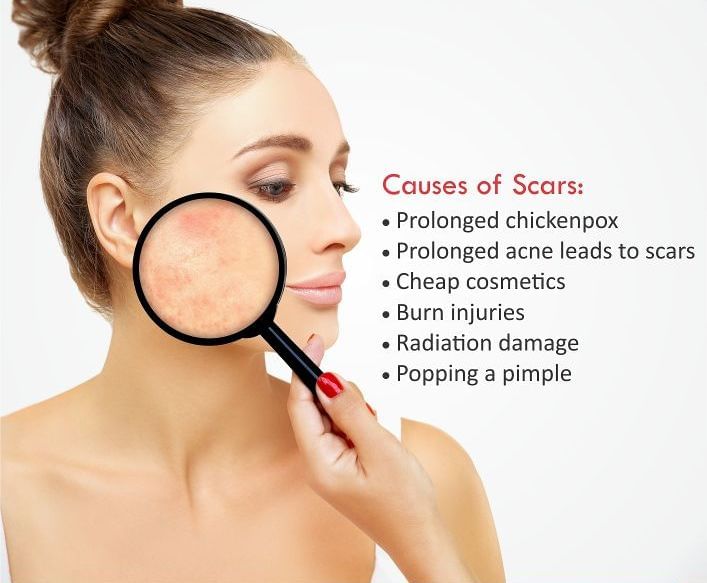
We all love that perfectly glowing skin that has no marks or signs of ageing like moles, tags, fine lines, dark circles and many others. However, for most of us, this remains an imaginary picture that we have in mind. What stares back at us in the mirror has some of the above-noted features, in various combinations. However, the desire for that blemish-free skin without any of these continues and is actually not far from reality too.
Some major irritants causing skin scars are as follow...more
Some major irritants causing skin scars are as follow...more
Last Updated: 6 years ago• Featured Tip
Share
Bookmark
Report
Over the last few decades, the demand for aesthetic procedures has escalated. Everyone wants to look the best. The skin can be ravaged over time, with age, exposure to the sun and rising levels of pollution. More and more people are willing to undergo treatment using energy based devices.
What is microneedle radiofrequency treatment?
Many forms of laser treatment leave scars on the skin and also have long-term side effects. But, Microneedle radio frequency is a highly efficient...more
What is microneedle radiofrequency treatment?
Many forms of laser treatment leave scars on the skin and also have long-term side effects. But, Microneedle radio frequency is a highly efficient...more
Last Updated: 6 years ago• Featured Tip
Share
Bookmark
Report
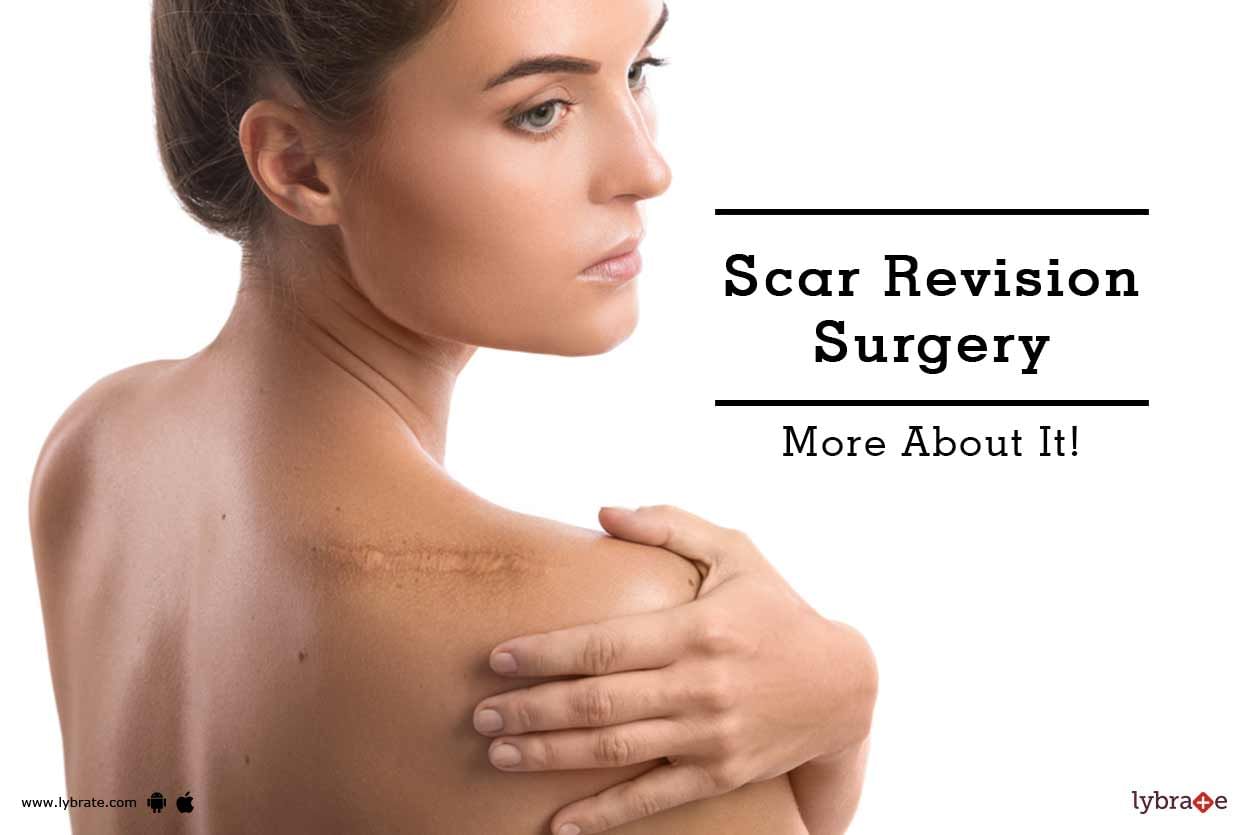
While some scars are negligible, others can mar your beauty. With cosmetic surgery, today, it is easy to remove scars and make them less prominent. Scar revision surgery can range from invasive procedures, such as scar excision to non-invasive procedures like cryotherapy, laser therapy and topical silicone therapy.
However, none of these has perfect results. The main aim of scar revision surgery is to make the scars blend in as much as possible with the surrounding skin in terms of colo...more
However, none of these has perfect results. The main aim of scar revision surgery is to make the scars blend in as much as possible with the surrounding skin in terms of colo...more
Last Updated: 6 years ago• Featured Tip
Share
Bookmark
Report
Almost everyone has scars on their body that tell tales of falls, accidents or surgeries. However, in some cases, these scars can mark a person s appearance and affect their self-confidence. In such cases, the person may consider scar revision surgery. As the name suggests, this surgery aims to minimise a scar and make it more consistent with the surrounding skin colour and texture. Anyone can undergo scar revision treatment. Some of the factors to be kept in mind while considering such treatmen...more
Last Updated: 6 years ago• Featured Tip
Share
Bookmark
Report
You may have heard a lot about teen acne and things related to it, especially its nature and solutions to cure this skin condition. However, there are several misconceptions about acne. Many facts regarding the cause and remedy for acne, which are commonly talked about, are incorrect. Here are some myths and facts about teen acne you should know about:
Tanning clears the skin: A tan may act as a temporary mask to prevent acne. However, the sun dries up the skin and irritates it. This ma...more
Tanning clears the skin: A tan may act as a temporary mask to prevent acne. However, the sun dries up the skin and irritates it. This ma...more
Last Updated: 7 years ago• Featured Tip
Share
Bookmark
Report
MS - General Surgery, MCh - Plastic Surg...read more
Cosmetic/Plastic Surgeon•Hyderabad
While some scars are negligible, others can mar your beauty. With cosmetic surgery, today, it is easy to remove scars and make them less prominent. Scar revision surgery can range from invasive procedures such as scar excision to non invasive procedures such as cryotherapy, laser therapy and topical silicone therapy. However, none of these have perfect results. The main aim of scar revision surgery is to make the scars blend in as much as possible with the surrounding skin in terms of colour, te...more
Last Updated: 7 years ago• Featured Tip
Share
Bookmark
Report
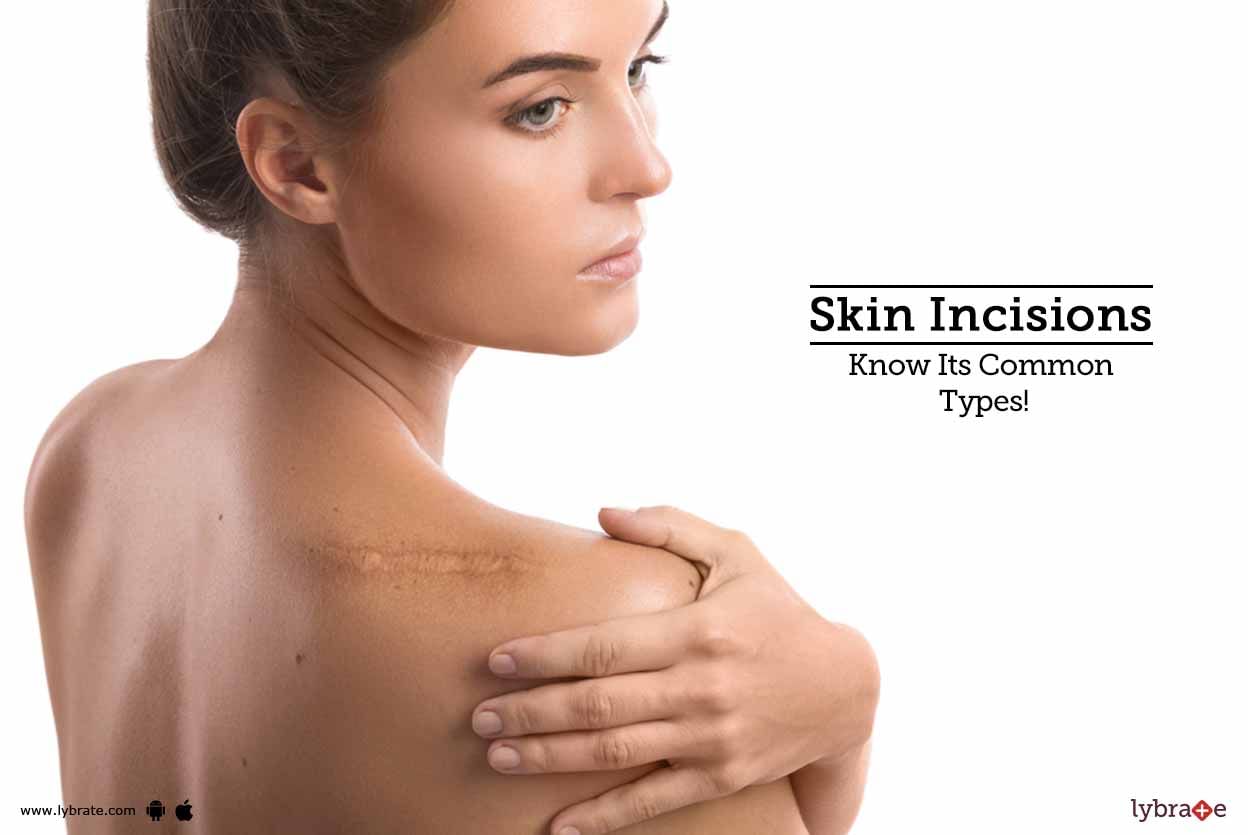
Ideally, surgical incisions are primarily designed to allow for easy access to the desired areas in addition to possibilities of extension, if required. Further, they should be designed to split muscles rather than cut them, with minimal scarring along with the aim of boosting regenerative and healing qualities.
Incisions can be classified under these three groups; vertical, transverse and oblique incisions.
Vertical Incision
1. Midline incision: Almost all abdominal i...more
Incisions can be classified under these three groups; vertical, transverse and oblique incisions.
Vertical Incision
1. Midline incision: Almost all abdominal i...more
Last Updated: 7 years ago• Featured Tip
Share
Bookmark
Report
Dermatologist•Delhi
Last Updated: 7 years ago• Featured Tip
Share
Bookmark
Report
Acne scars are caused when a pimple or cyst is popped and broken leaving a layer of damaged skin behind. Acne (pimples) are caused by the excess oil, dead skin, and bacteria blocking the skin pores causing it to swell.
Causes of Acne(pimples):
Acne and acne scars can be caused due to the following reasons:
Hormonal imbalance during or after the onset of puberty
Medicines that contains lithium, androgen or corticosteroids
Oil and greasy food items and those...more
Causes of Acne(pimples):
Acne and acne scars can be caused due to the following reasons:
Hormonal imbalance during or after the onset of puberty
Medicines that contains lithium, androgen or corticosteroids
Oil and greasy food items and those...more
Book appointment with top doctors for Skin Scars treatment
View fees, clinic timings and reviews
Ask a free question
Get FREE multiple opinions from Doctors
posted anonymously