Get the App
For Doctors
Login/Sign-up
Health Feed
Find Doctors
Health Packages
AllQ&AsTipsQuizzes
Reconstructive Health Feed
Last Updated: 5 years ago• Featured Tip
Share
Bookmark
Report
MBBS Bachelor of Medicine and Bachelor o...read more
Orthopedic Doctor•Bhubaneswar
The anterior cruciate ligament (acl) is a rope like connective tissue that gives support and stability to the knee, along with other related tissues. If you do not repair it, you can still perform many functions, and carry on with your life with little difficulty. However, surgery to correct the ligament tear is recommended if you do not want the injury to impede your sporting activities and want a 100% normal knee.
The acl reconstruction surgery can be performed in two ways, the arthro...more
The acl reconstruction surgery can be performed in two ways, the arthro...more
Last Updated: 5 years ago• Featured Tip
Share
Bookmark
Report
Skin graft is a form of a surgical procedure, which involves removal of the skin of a particular region of the body and transplanting it to a different body portion or to a separate individual. Grafting is usually recommended by the doctor if the patient has suffered from extreme burns or the protective layering of the skin of that particular region has been damaged because of extreme illness, bed sores sustained infection on the skin or repeated injuries. Grafting is also recommended as a proce...more
Last Updated: 6 years ago• Featured Tip
Share
Bookmark
Report
Craniofacial surgery is required when there are deformities or abnormalities present in the head or face area of the patient. Depending on the type of deformity, a craniofacial surgery is done to repair or reconstruct it.
The areas that come under a craniofacial surgeon's domain are the cranium (skull), the brain, the face, skin on the face, facial bones, and the nerves. For this reason, in order to conduct craniofacial surgery, a neurosurgeon and a cosmetic surgeon may often work toget...more
The areas that come under a craniofacial surgeon's domain are the cranium (skull), the brain, the face, skin on the face, facial bones, and the nerves. For this reason, in order to conduct craniofacial surgery, a neurosurgeon and a cosmetic surgeon may often work toget...more
Last Updated: 6 years ago• Featured Tip
Share
Bookmark
Report
MCh, MS - General Surgery, MBBS Bachelor...read more
Cosmetic/Plastic Surgeon•Faridabad
Burn surgery is very common these days. Burn surgery is usually done on people who suffer from major burns. Reconstructive burn surgery is usually required in the last stages when the initial burns have healed to a certain extent. Usually, reconstructive burn surgeries are done on patients who have suffered from huge accidents and have burnt their face, neck and hands to a great extent. Patients requiring this surgery usually become unrecognizable after an accident.
When is reconstructi...more
When is reconstructi...more
Last Updated: 6 years ago• Featured Tip
Share
Bookmark
Report
Ulcers and perforations of cornea are some very serious clinical conditions, which threaten vision rapidly and progressively, and disintegrate the eye globe. They need to be taken care of immediately to prevent irreparable damage to the eyes. In spite of the advanced medical research and practice, severe injuries, infections, and diseases of cornea can lead to serious corneal perforations, which require surgery necessarily as the ultimate solution.
Urgent reconstructive surgery might be...more
Urgent reconstructive surgery might be...more
Last Updated: 6 years ago• Featured Tip
Share
Bookmark
Report
MCh - Plastic and Reconstructive Surgery...read more
Cosmetic/Plastic Surgeon•Hyderabad
A cleft palate and cleft lip are among the most common congenital birth defects. These conditions can occur individually or together and vary in severity and the side of the face affected. A cleft palate not only mars the beauty of a child, but can also lead to serious health problems associated with speech and food intake.
A cleft palate can be diagnosed in the 17th week of pregnancy with the help of an ultrasound. This condition develops when components of the upper lip and ceiling of...more
A cleft palate can be diagnosed in the 17th week of pregnancy with the help of an ultrasound. This condition develops when components of the upper lip and ceiling of...more
Last Updated: 6 years ago• Featured Tip
Share
Bookmark
Report
Contrary to what most girls have been led to believe about the hymen being a flat tissue that covers the vagina and is ripped during penetrative sex, the truth is that hymen is a fringe of tissue around the vaginal opening. It is not an intact tissue draping across the vaginal wall because, without any outlet for the menstrual blood, girls would get periods only after they lose their virginity.
Here are a few mind-boggling facts about the hymen.
1. Just like labia, every woman...more
Here are a few mind-boggling facts about the hymen.
1. Just like labia, every woman...more
Last Updated: 6 years ago• Featured Tip
Share
Bookmark
Report
Hymnoplasty is also known as hymen surgery. It is a surgical procedure where the hymen within the vagina is restored. The Hymen is a membrane covering the vaginal opening, which can be torn when a woman engages in coitus for the first time or it could be damaged due to other factors such as heavy lifting, exercise, cycling, swimming among many other activities. Hymnoplasty involves putting back the hymen s torn edges to make it look like the hymen is intact.
Why do women want hymen reco...more
Why do women want hymen reco...more
Last Updated: 6 years ago• Featured Tip
Share
Bookmark
Report
DNB (Plastic Surgery), DNB General Surge...read more
Cosmetic/Plastic Surgeon•Pune
Facial surgery can be opted by people for a number of reasons, and these include being born with facial impairments like cleft lip, birthmark or other birth defects, the effects of aging, sun damage or other facial traumas that are noticeable on the face as well as a sense of general dissatisfaction with your facial features. Depending on these factors, facial plastic surgery can be divided into two categories - reconstructive and cosmetic.
Reconstructive plastic surgery is performed fo...more
Reconstructive plastic surgery is performed fo...more
Last Updated: 6 years ago• Featured Tip
Share
Bookmark
Report
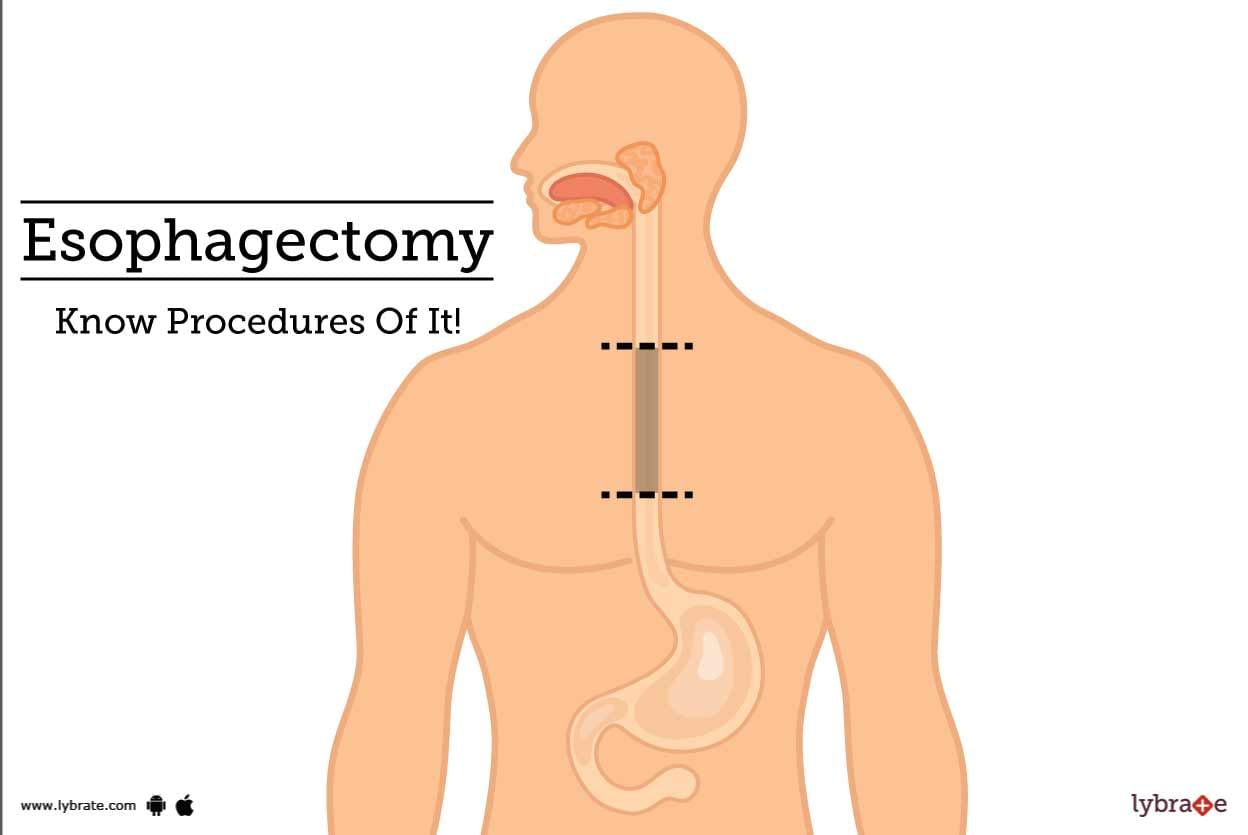
The surgical procedure to remove the oesophagus (the tube between your stomach and mouth), partially or completely, and reconstruct it by using a section of the large intestine or stomach is called esophagectomy.
Esophagectomy is commonly used to treat oesophageal cancer.
Uses:
Early-stage oesophageal cancer is frequently treated with an esophagectomy. Other than that, esophagectomy is also performed to treat oesophageal dysplasia (a condition in which cells in the oes...more
Esophagectomy is commonly used to treat oesophageal cancer.
Uses:
Early-stage oesophageal cancer is frequently treated with an esophagectomy. Other than that, esophagectomy is also performed to treat oesophageal dysplasia (a condition in which cells in the oes...more
Book appointment with top doctors for Reconstructive treatment
View fees, clinic timings and reviews
Ask a free question
Get FREE multiple opinions from Doctors
posted anonymously