Get the App
For Doctors
Login/Sign-up
Health Feed
Find Doctors
Health Packages
AllQ&AsTipsQuizzes
Prophylaxis For Deep Vein Thrombosis Tips
Last Updated: 6 years ago• Featured Tip
Share
Bookmark
Report
Multi Speciality•Chandigarh
Peripheral vascular disease (PVD) is a circulation issue that affects the veins and blood vessels outside of the brain and heart. PVD commonly strikes the veins that supply blood to the arms, legs, and organs situated beneath the stomach. These are the veins that are located away from the heart. They are known as peripheral vessels.
In PVD, the width of the veins get limited. Narrowing is normally created by arteriosclerosis. Arteriosclerosis is a condition where plaque develops inside ...more
In PVD, the width of the veins get limited. Narrowing is normally created by arteriosclerosis. Arteriosclerosis is a condition where plaque develops inside ...more
Last Updated: 6 years ago• Featured Tip
Share
Bookmark
Report
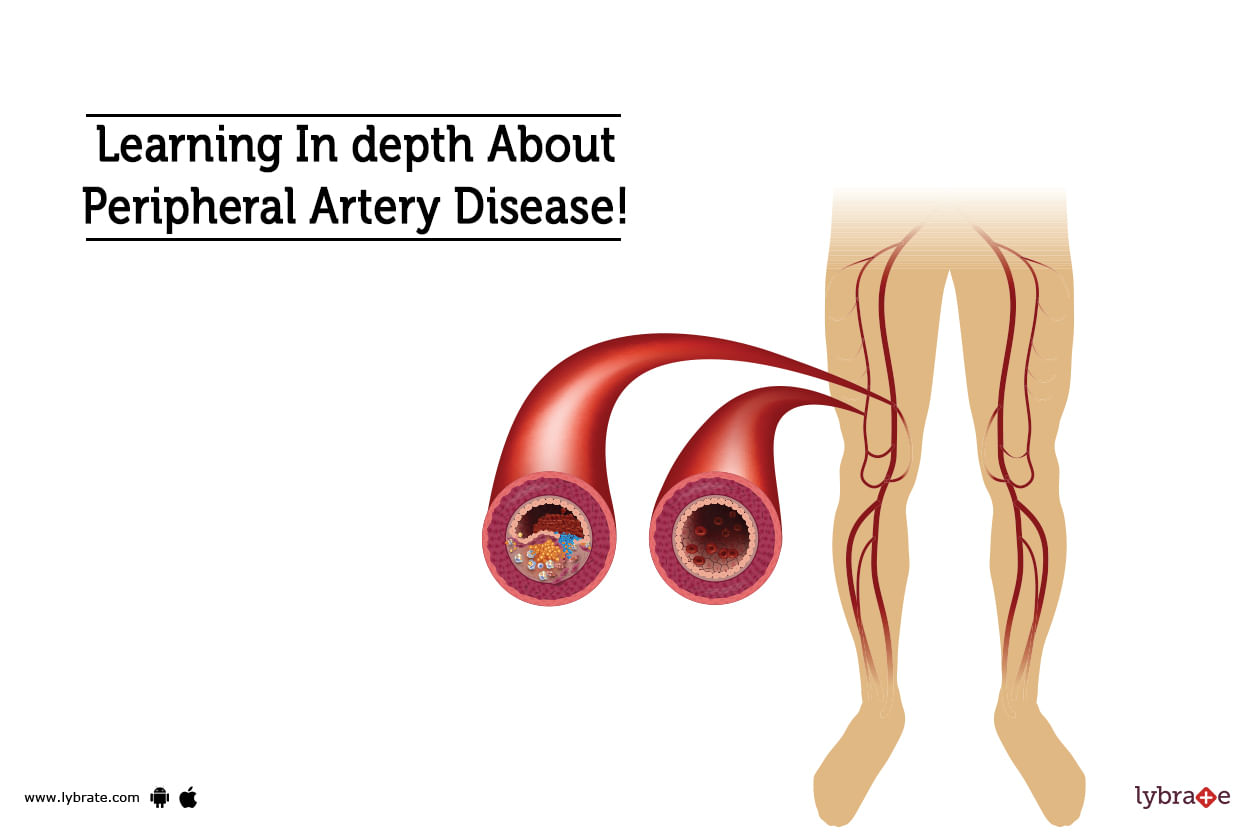
Peripheral Artery Disease (PAD) is a disease of blood vessels that are located outside the heart and brain. The condition develops due to fatty deposits in the arteries and veins that stops the blood flow to the heart and mind as the case may be. It narrows the artery and restricts the blood flow, which causes problems to other organs of the body such as kidney, liver, and stomach.
Symptoms of Peripheral Artery Disease-
Peripheral Artery Disease is the most common type of condi...more
Symptoms of Peripheral Artery Disease-
Peripheral Artery Disease is the most common type of condi...more
Last Updated: 6 years ago• Featured Tip
Share
Bookmark
Report
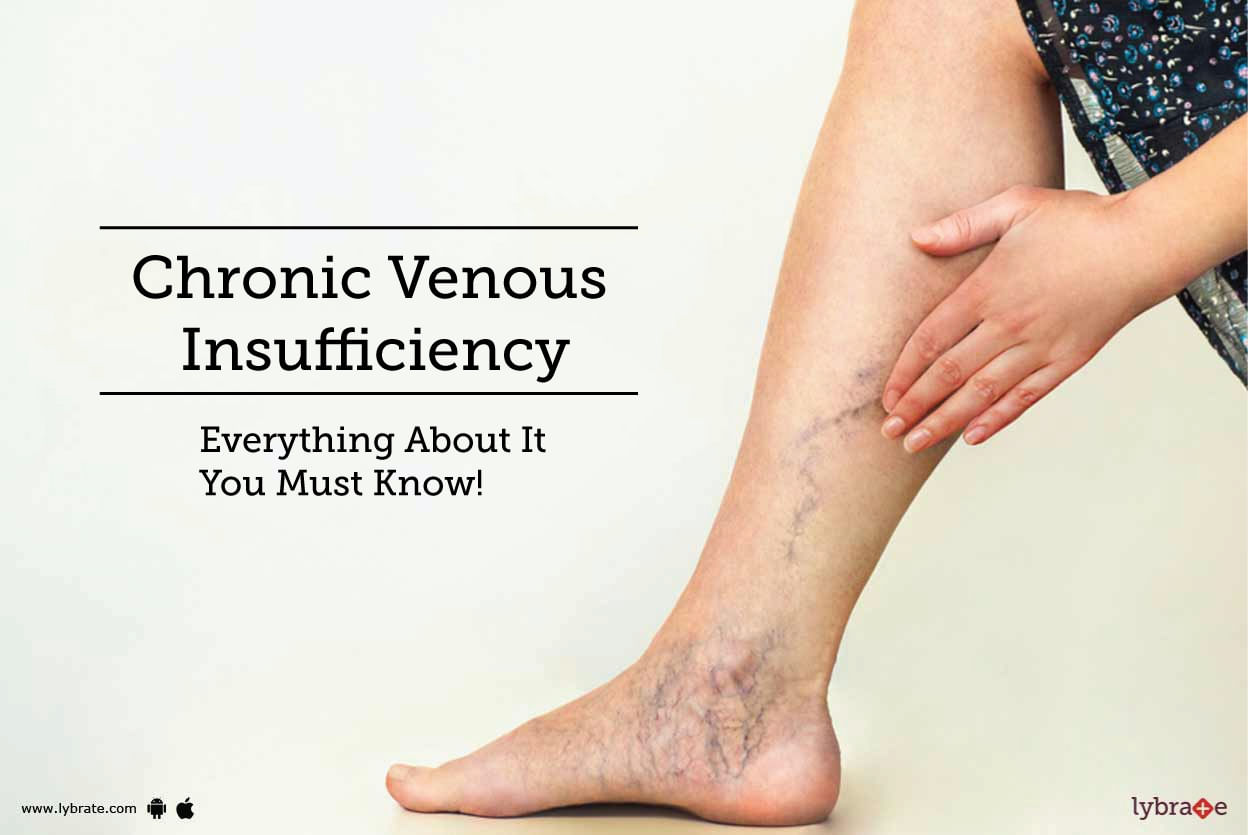
Chronic Venous Insufficiency is an abnormal condition of the leg veins. It occurs when either the walls or the one-way valves of the veins cannot work effectively. This
makes it difficult for the veins to send the impure blood from the legs to the heart. This results in impure flowing backward and collecting at places in the veins. It can
cause swelling, pain, and changes in skin and over time may lead to ulcers in legs.
Causes of Chronic Venous Insufficiency
Veins retu...more
makes it difficult for the veins to send the impure blood from the legs to the heart. This results in impure flowing backward and collecting at places in the veins. It can
cause swelling, pain, and changes in skin and over time may lead to ulcers in legs.
Causes of Chronic Venous Insufficiency
Veins retu...more
Last Updated: 6 years ago• Featured Tip
Share
Bookmark
Report
Food is one of the most common ways of getting an infection, and so the stomach is more prone to infections than other body parts. Whether it is eating raw or uncooked foods or unhygienic foods, the stomach bears the brunt of one s bad food practices. The only consoling factor is that it is equally easy to treat a stomach infection if some simple measures are adhered to.
Read on to know some of the easiest and most effective ways to treat a stomach infection.
Drink it right: Wh...more
Read on to know some of the easiest and most effective ways to treat a stomach infection.
Drink it right: Wh...more
Last Updated: 6 years ago• Featured Tip
Share
Bookmark
Report
Carotid artery disease occurs when an oily, waxy substance called plaque builds up inside the carotid arteries. These are arteries that supply oxygenated blood to your brain, face, scalp, and neck.
Carotid artery disease is very serious as it can cause a brain stroke. It, in fact, starts with damage to the inner layer of the carotid artery. To stem this damage your body starts a healing process and this leads to a build up of plaque at the point where the artery is damaged.
When thi...more
Carotid artery disease is very serious as it can cause a brain stroke. It, in fact, starts with damage to the inner layer of the carotid artery. To stem this damage your body starts a healing process and this leads to a build up of plaque at the point where the artery is damaged.
When thi...more
Last Updated: 6 years ago• Featured Tip
Share
Bookmark
Report
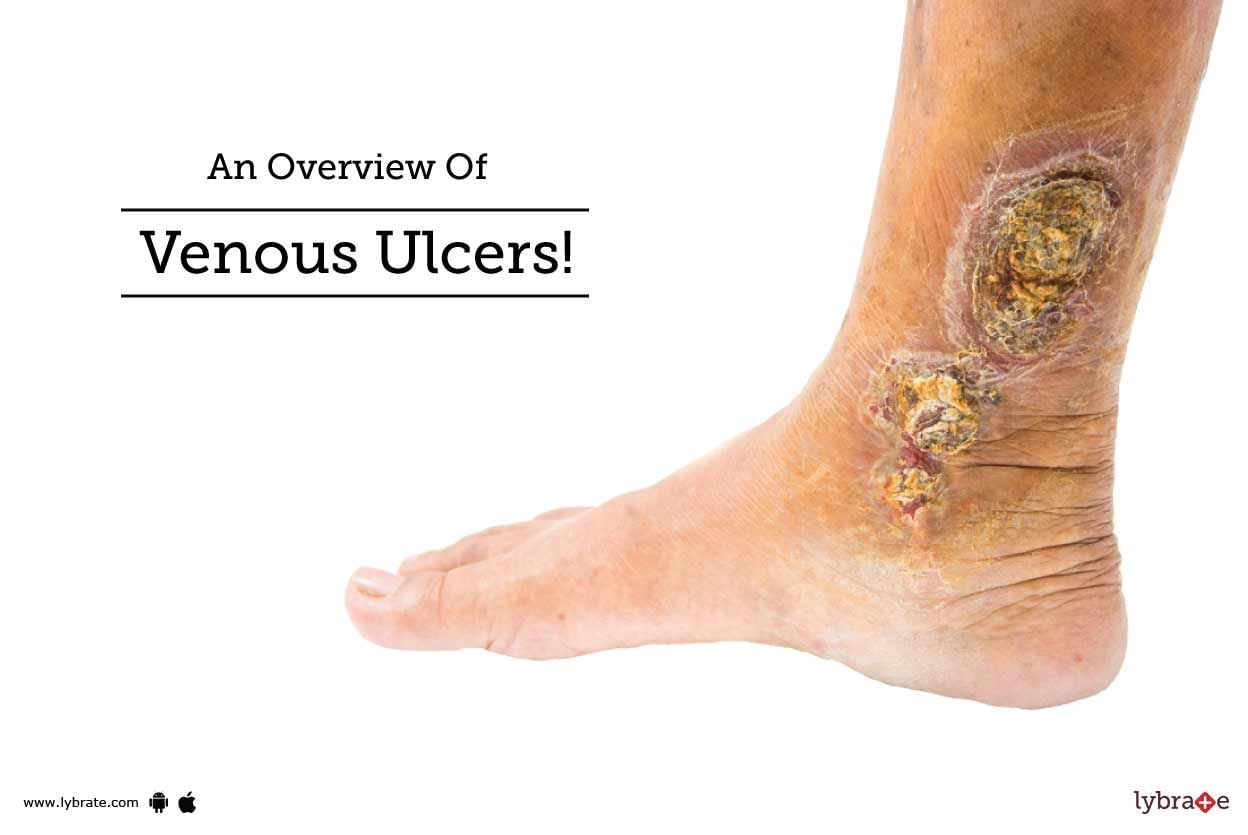
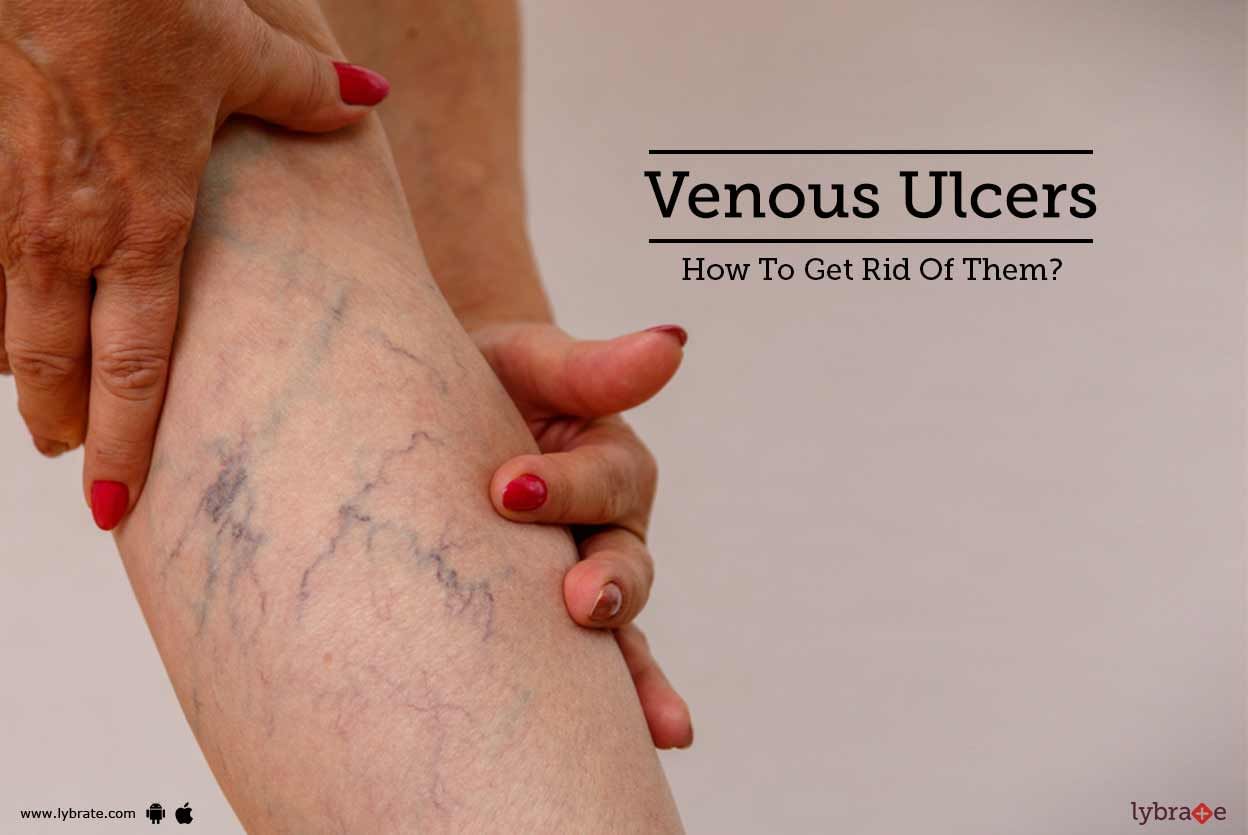
Venous Ulcers are also known as venous skin ulcers. They are nothing but slow-healing sores on legs that primarily result from weak blood circulation to the limbs. Such ulcers may last a few weeks or even years. However, one needs to get them treated since it may worsen the problem.
What Causes Venous Ulcers?
It may happen if there is a break in the skin around one of the ankles. The leg veins, which send impure blood to the heart may become weak and not work well enough. In most ca...more
What Causes Venous Ulcers?
It may happen if there is a break in the skin around one of the ankles. The leg veins, which send impure blood to the heart may become weak and not work well enough. In most ca...more
Last Updated: 6 years ago• Featured Tip
Share
Bookmark
Report
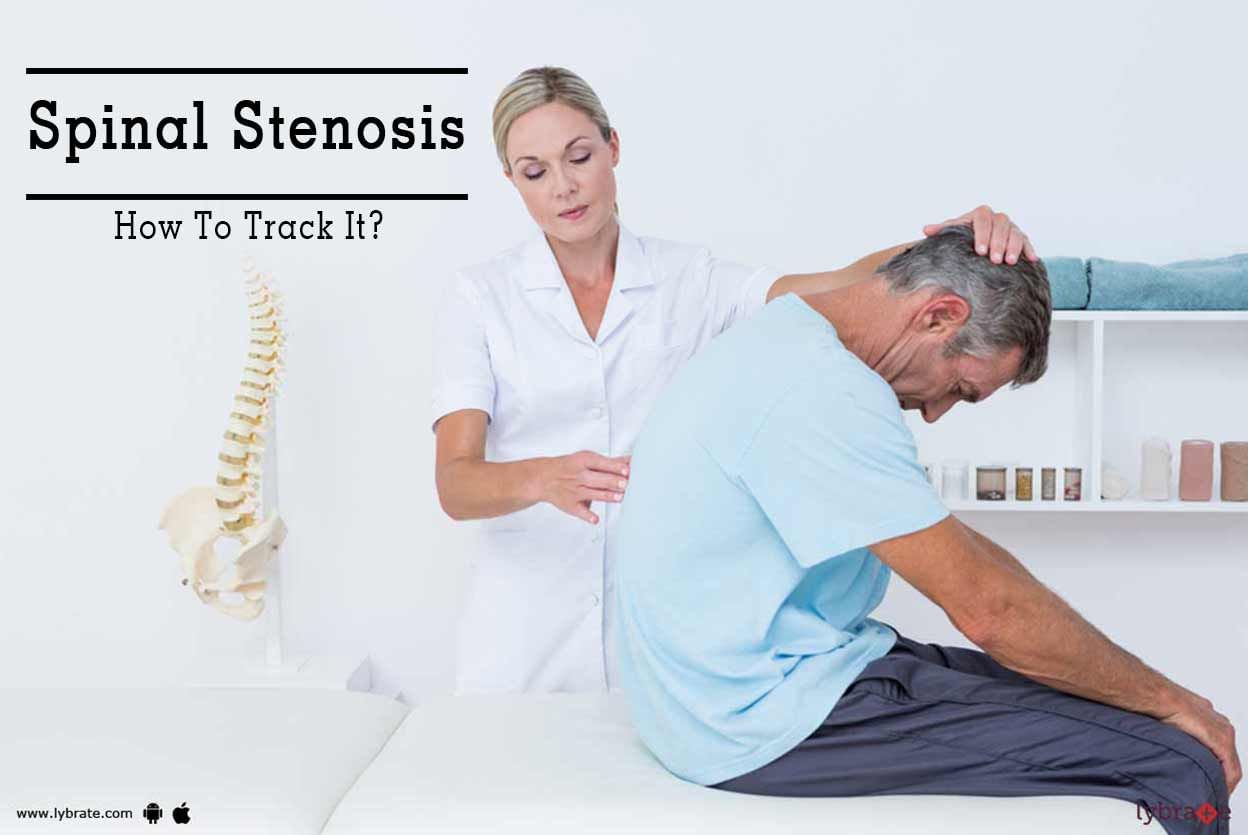
What is Spinal Stenosis: The narrowing of the gaps in the spine or the backbone is called as Spinal stenosis. This leads to pressure on the nerves and the spinal cord. 5% of cases of spinal stenosis are seen in the low back of the lumbar spine. In some cases the narrowing of the spine leads to the compressing of the nerve root, which leads to pain in the leg.
Causes of spinal stenosis: It can be caused by aging, arthritis, trauma to the spine, spondylolisthesis and tumor of the spinemore
Causes of spinal stenosis: It can be caused by aging, arthritis, trauma to the spine, spondylolisthesis and tumor of the spine
Last Updated: 6 years ago• Featured Tip
Share
Bookmark
Report
Venous Ulcers are also known as venous skin ulcers. They are nothing but slow-healing sores on legs that primarily result from weak blood circulation to the limbs. Such ulcers may last a few weeks or even years. However, one needs to get them treated since it may worsen the problem.
What Causes Venous Ulcers?
It may happen if there is a break in the skin around one of the ankles. The leg veins, which send impure blood to the heart may become weak and not work well enough. In most ca...more
What Causes Venous Ulcers?
It may happen if there is a break in the skin around one of the ankles. The leg veins, which send impure blood to the heart may become weak and not work well enough. In most ca...more
Last Updated: 6 years ago• Featured Tip
Share
Bookmark
Report
Spinal stenosis is a condition where a part of the spinal column becomes narrow. There are generally two types of spinal stenosis- lumbar stenosis and cervical stenosis. Lumbar stenosis is the form of the condition that affects the lower back. It is also the most common type of spinal stenosis.
Common Causes of Lumbar Spinal Stenosis
Some people may be born with a narrow spinal canal, but in most cases the condition is caused post birth. Here is a look at some of the most common cau...more
Common Causes of Lumbar Spinal Stenosis
Some people may be born with a narrow spinal canal, but in most cases the condition is caused post birth. Here is a look at some of the most common cau...more
Last Updated: 6 years ago• Featured Tip
Share
Bookmark
Report
Pulmonary edema is a disorder wherein fluid accumulates in the lungs leading to lack of oxygen in the body. The usual cause of pulmonary edema is congestive heart failure (the muscles of the heart are unable to pump blood). In this disorder, the heart has to work extra hard to pump blood, so this adds extra pressure on the blood vessels that are present in the lungs. In a bid to relieve this added pressure, fluid is released into the lungs by the blood vessels.
The function of your lung...more
The function of your lung...more
Book appointment with top doctors for Prophylaxis For Deep Vein Thrombosis treatment
View fees, clinic timings and reviews
Ask a free question
Get FREE multiple opinions from Doctors
posted anonymously