Get the App
For Doctors
Login/Sign-up
About
Health Feed
Find Doctors
Health Packages
AllQ&AsTipsQuizzes
Physiotherapy Tips
Last Updated: 3 years ago• Featured Tip
Share
Bookmark
Report
1. Dr. Ashutosh sharma
Https://www. Lybrate. Com/delhi/doctor/dr-ashutosh-sharma-ayurveda ;
Bachelor of ayurveda, medicine and surgery (bams)
19 years experience 200 at clinic 350 online
He is a well respected physician having a number of patients treated with complex issues. He has earned his prestigious education and clinical expertise as an ayurvedic doctor. He has massive experience as an orthopedist. He has obtained b...more
204 people found this helpful
Last Updated: 5 years ago• Featured Tip
Share
Bookmark
Report
Without our lungs, it would be impossible to breathe. People suffering from chronic lung diseases have compromised lung functioning. This leads to shortness of breath, fatigue and weakness. In turn, this can make the person avoid anything that exerts the lungs such as exercise. While this may seem like a good idea, it is actually detrimental. Not exercising can further weaken the lungs and muscles and make this a vicious cycle. This is where physiotherapy can help with lung rehabilitation or pul...more
Last Updated: 5 years ago• Featured Tip
Share
Bookmark
Report
B.P.T, M.P.T, Fellowship In Cardiac Reha...read more
Physiotherapist•Bangalore
Seeing someone who used to do all their activities on their own turn to someone who needs help even with small things like going to the bathroom can be very difficult.
The lungs are vital organs in that they are essential to supply oxygen to the entire body. If the various organs do not receive adequate oxygen, their function can be impaired. Therefore, lung function needs to be maintained. Lung function can be impaired by chronic conditions like COPD and bronchiectasis. In both these, ...more
The lungs are vital organs in that they are essential to supply oxygen to the entire body. If the various organs do not receive adequate oxygen, their function can be impaired. Therefore, lung function needs to be maintained. Lung function can be impaired by chronic conditions like COPD and bronchiectasis. In both these, ...more
Last Updated: 6 years ago• Featured Tip
Share
Bookmark
Report
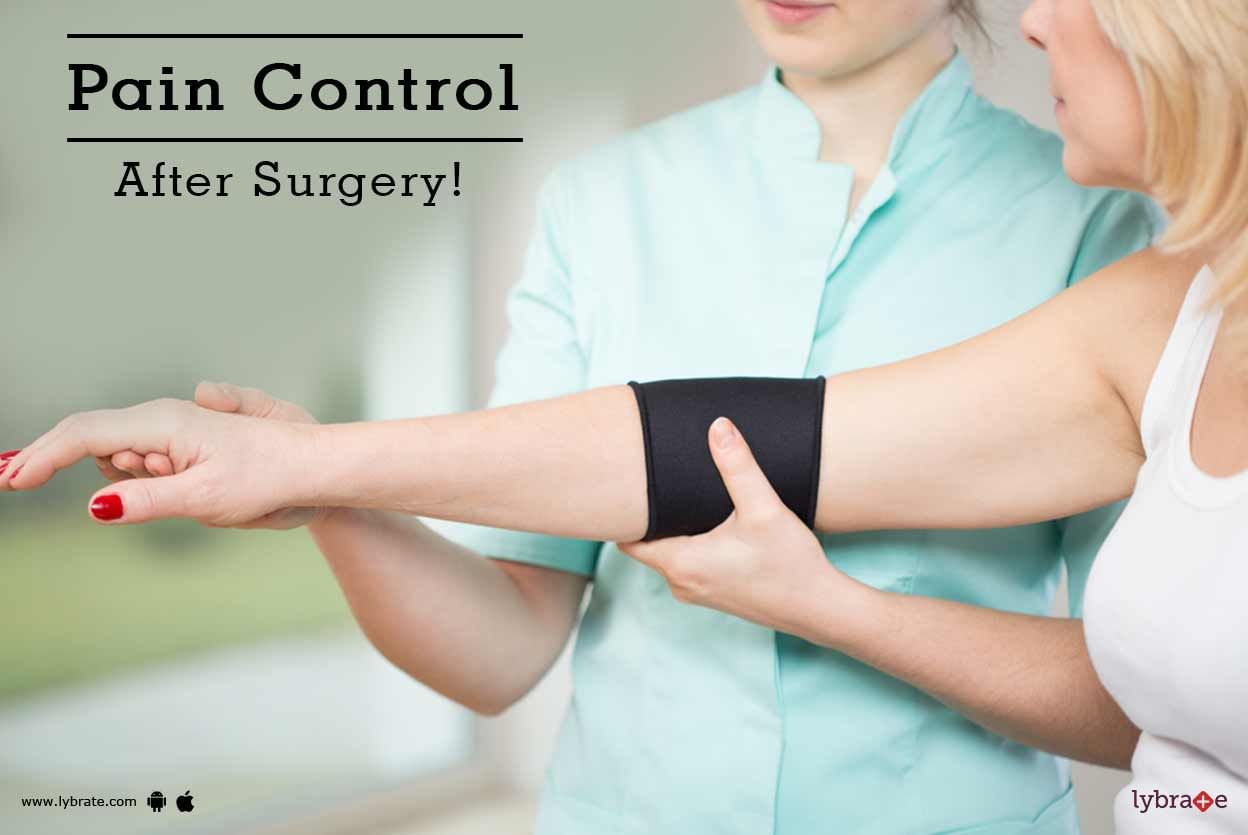
The word 'surgery' is often dreaded by most patients. Be it an invasive oral surgery or a keyhole gallbladder surgery, it does not evoke a ready "yes" in most patients. There are too many patients who are ready to be on long-term medications if they could avoid the surgery and its complications. While there could be swelling, bruising, tingling, and many other symptoms, the one feared by most is the postoperative pain. What happens after the effect of the anesthetic wears off can leave many pati...more
Last Updated: 6 years ago• Featured Tip
Share
Bookmark
Report
Clinical Fellowship In Pain Management, ...read more
Pain Management Specialist•Hyderabad
Lower back pain is fast becoming an epidemic not just among the elderly, but across all age groups. Primary causes of back pain are quite a few including lumbar hernia, disc degenerative disease (DDD), spondylosis etc., but the symptoms are usually the same excruciating pain in the lower region of the spine, followed by stiffness. Since back pain is caused due to a number of spinal problems, it manifests differently in different patients. The pain may be dull, burning or sharp. It could also be ...more
Last Updated: 6 years ago• Featured Tip
Share
Bookmark
Report
Tennis Elbow is involved with the muscles and tendons of one s forearm. It leads to inflammation of the tendons which join the forearm muscles on the outside of the elbow. Physiotherapy treatment can be of great help. The primary goal of this treatment is to improve the strength as well as the flexibility of one's forearm muscles. Now, before we take a look at the tips regarding physiotherapy treatment, let us briefly discuss its symptoms and causes.
Symptoms
If a person suffer...more
Symptoms
If a person suffer...more
Last Updated: 6 years ago• Featured Tip
Share
Bookmark
Report
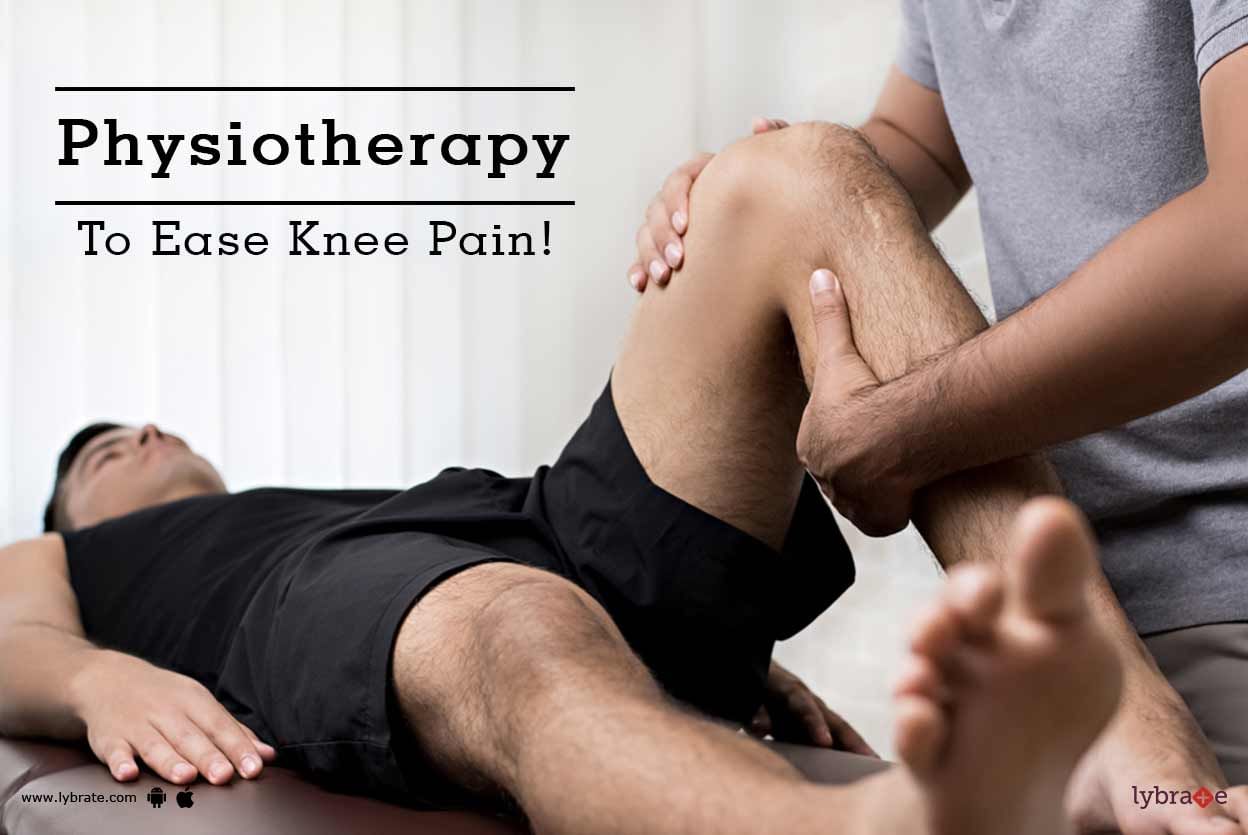
Knee pain is one of the most common and painful ailments that can limit mobility. Injuries can result in cartilage or meniscal tears or sprains too. Obesity is another reason knee pain is on the rise. Also, regular wear and tear of the ligaments and tendons around the knees due to old age is another cause. These days, with reduced physical activities and sedentary lifestyles, the rate at which knees are wearing out has also become accelerated. Whatever the reason, a correct diagnosis followed...more
Last Updated: 6 years ago• Featured Tip
Share
Bookmark
Report
What is physiotherapy?
Physiotherapy helps to improve the strength of muscle, and joint which is affected by injury, diseases, or disability through movement, exercise, manual therapy, and advice.
What are the most common joint complaints?
Rheumatoid arthritis, osteoarthritis, and gout are the most common complaint, and physiotherapy has a great role in it.
What are the benefits of physiotherapy in joint complaints?
It reduces pain which in turn helps you redu...more
Physiotherapy helps to improve the strength of muscle, and joint which is affected by injury, diseases, or disability through movement, exercise, manual therapy, and advice.
What are the most common joint complaints?
Rheumatoid arthritis, osteoarthritis, and gout are the most common complaint, and physiotherapy has a great role in it.
What are the benefits of physiotherapy in joint complaints?
It reduces pain which in turn helps you redu...more
Last Updated: 6 years ago• Featured Tip
Share
Bookmark
Report
World cerebral palsy day is celebrated on October 6. Cerebral palsy refers to a medical condition where a child suffers from certain disabilities as a result of damage caused to his or her brain during or before birth. If a child is diagnosed with cerebral palsy then he or she may experience a problem with body movement and brain development may also get affected. Along with difficulties in body movements, there are many other problems that he or she may encounter, such as difficulties in hearin...more
Last Updated: 6 years ago• Featured Tip
Share
Bookmark
Report
Physiotherapist•Hyderabad
Chronic Obstructive Pulmonary Disease, abbreviated as COPD, is an umbrella term which refers to the group of lung infections and diseases that include emphysema, chronic bronchitis, and diseases of the small airways. Most people feel breathlessness, which is caused due to impairment of gaseous exchange that happens because of prolonged damage to the lungs over a period of time.
Symptoms such as fatigue, reduced tolerance to exercise, muscular dysfunction, breathlessness even after simpl...more
Symptoms such as fatigue, reduced tolerance to exercise, muscular dysfunction, breathlessness even after simpl...more
Book appointment with top doctors for Physiotherapy treatment
View fees, clinic timings and reviews
Ask a free question
Get FREE multiple opinions from Doctors
posted anonymously