Get the App
For Doctors
Login/Sign-up
Health Feed
Find Doctors
Health Packages
AllQ&AsTipsQuizzes
Dental Prophylaxis Tips
Last Updated: 3 years ago• Featured Tip
Share
Bookmark
Report
Dr. Anupam Agarwal
MDS - Orthodontics
14 Years Experience 500 at clinic 800 online
He's been practising dentistry for 14 years and has an excellent reputation as a specialist in his area. He is able to identify and treat a broad variety of complex diseases because to his ability to draw from several fields of study. Due to his dual professions as an Orthodontist and Cosmetic Dentist, he has extensive experience using Laser Therapy on his patients.
He attended the repu...more
MDS - Orthodontics
14 Years Experience 500 at clinic 800 online
He's been practising dentistry for 14 years and has an excellent reputation as a specialist in his area. He is able to identify and treat a broad variety of complex diseases because to his ability to draw from several fields of study. Due to his dual professions as an Orthodontist and Cosmetic Dentist, he has extensive experience using Laser Therapy on his patients.
He attended the repu...more
Last Updated: 3 years ago• Featured Tip
Share
Bookmark
Report
Did you recently get clear aligners, or are you still thinking about it? in the past few years, orthodontic treatment has transformed greatly. Gone are the days when orthodontic treatment meant metal braces, cuts on cheeks, and uncomfortably smiling for photographs. With clear aligners, you can get a perfect smile without any aesthetic repercussions.
;
Whether you ve already started your treatment or are still considering it, the following tips will be bene...more
Last Updated: 3 years ago• Featured Tip
Share
Bookmark
Report
1. Dr. Manjunath B.S.
BDS, MDS-PROSTHODONTICS
28 years experience 500 at clinic 500 online
If someone looks for one of the top dentists in Bangalore, a familiar name that comes to mind is Dr. Manjunath B.S. He is a well-known dentist in Bangalore's Jayanagar district. He earned degrees in M.D.S. Prosthodontics and B.D.S. He has 28 years of successful experience as a dentist and is currently working at the Ramitha dental clinic in Bangalore's Jayanagar region. He offers cutting-...more
BDS, MDS-PROSTHODONTICS
28 years experience 500 at clinic 500 online
If someone looks for one of the top dentists in Bangalore, a familiar name that comes to mind is Dr. Manjunath B.S. He is a well-known dentist in Bangalore's Jayanagar district. He earned degrees in M.D.S. Prosthodontics and B.D.S. He has 28 years of successful experience as a dentist and is currently working at the Ramitha dental clinic in Bangalore's Jayanagar region. He offers cutting-...more
7 people found this helpful
Last Updated: 3 years ago• Featured Tip
Share
Bookmark
Report
1. Dr. Amruta Kakade Tamhankar
B.D.S.
19 Years Experience 500 At Clinic 500 Online
He is an expert in therapy, including dental medicine, radiology, and Cosmetic/ Aesthetic Dentistry, and his expert skills as a prosthodontist were acquired from Pune University's B.D.S. programme in 2003. skilled proprietor of All Care Dental Clinic.
He is BNI's regional director and a trusted Dentist working in Karmoli, Pune. She has been a successful dentist for the past 19 years.
more
B.D.S.
19 Years Experience 500 At Clinic 500 Online
He is an expert in therapy, including dental medicine, radiology, and Cosmetic/ Aesthetic Dentistry, and his expert skills as a prosthodontist were acquired from Pune University's B.D.S. programme in 2003. skilled proprietor of All Care Dental Clinic.
He is BNI's regional director and a trusted Dentist working in Karmoli, Pune. She has been a successful dentist for the past 19 years.
more
3 people found this helpful
Last Updated: 3 years ago• Featured Tip
Share
Bookmark
Report
Dr. Devaanshu dewan
Https://www. Lybrate. Com/delhi/doctor/dr-devaanshu-dewan-dentist
Bds (implantologist)
;
Dr. Devaanshu dewan is a prominent dentist in uttam nagar, delhi. During his 17 years of expertise in dentistry, he has been of assistance to a significant number of patients in the areas of dental surgery and implantology. In 2005, he graduated with a bachelor of dental surgery degree from the subharti dental college in meerut.
In 2019, he ...more
Https://www. Lybrate. Com/delhi/doctor/dr-devaanshu-dewan-dentist
Bds (implantologist)
;
Dr. Devaanshu dewan is a prominent dentist in uttam nagar, delhi. During his 17 years of expertise in dentistry, he has been of assistance to a significant number of patients in the areas of dental surgery and implantology. In 2005, he graduated with a bachelor of dental surgery degree from the subharti dental college in meerut.
In 2019, he ...more
Last Updated: 5 years ago• Featured Tip
Share
Bookmark
Report
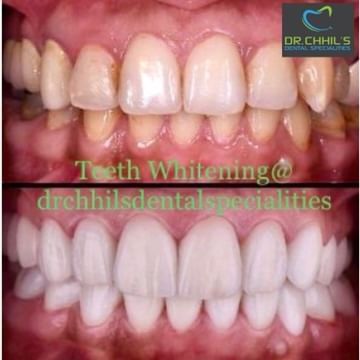
Many people turn to teeth whitening treatments to achieve a whiter smile either professionally or in the comfort of their own homes. While the treatment itself is crucial to get the result you dream of, what you do afterwards is equally important to keep your teeth white.
Foods to avoid after teeth whitening treatment
Going through the procedure will cost you money, so you would want to make sure the stunning result will last a long time. The first 48 hours after the treatment is cr...more
Foods to avoid after teeth whitening treatment
Going through the procedure will cost you money, so you would want to make sure the stunning result will last a long time. The first 48 hours after the treatment is cr...more
Last Updated: 5 years ago• Featured Tip
Share
Bookmark
Report
M.Sc. in Dietetics and Food Service Mana...read more
Dietitian/Nutritionist•Mumbai
Last Updated: 5 years ago• Featured Tip
Share
Bookmark
Report
Last Updated: 5 years ago• Featured Tip
Share
Bookmark
Report
Dental care that you should have taken care of by a dentist at this covid-19 time:
1- bleeding that doesn t stop
2- painful swelling in or around your mouth
3- pain in a tooth, teeth or jaw bone
4- gum infection with pain or swelling
5- after surgery treatment (dressing change, stitch removal)
6- broken or knocked out tooth
7- denture adjustment for people receiving radiation or other treatment for cancer
8- snipping or adjusting wire of braces that hu...more
1- bleeding that doesn t stop
2- painful swelling in or around your mouth
3- pain in a tooth, teeth or jaw bone
4- gum infection with pain or swelling
5- after surgery treatment (dressing change, stitch removal)
6- broken or knocked out tooth
7- denture adjustment for people receiving radiation or other treatment for cancer
8- snipping or adjusting wire of braces that hu...more
Last Updated: 5 years ago• Featured Tip
Share
Bookmark
Report
Dentist•Arrah
Book appointment with top doctors for Dental Prophylaxis treatment
View fees, clinic timings and reviews
Ask a free question
Get FREE multiple opinions from Doctors
posted anonymously