Get the App
For Doctors
Login/Sign-up
Health Feed
Find Doctors
Health Packages
AllQ&AsTipsQuizzes
Cartilage Surgery Tips
Last Updated: 6 years ago• Featured Tip
Share
Bookmark
Report
What is Articular Cartilage Injury?
Cartilage is an important structural unit of the body. It is present in places like the joints, the spine, the end of ribs, in the bronchial tubes, and the ear and the nose. Cartilages are firm, but flexible tissues. There are many types of cartilages found in the body. Among them, articular cartilages are the ones that are present on the surface of the bones. As the name suggests articular cartilages exist to render articulation to the bones and retain t...more
Cartilage is an important structural unit of the body. It is present in places like the joints, the spine, the end of ribs, in the bronchial tubes, and the ear and the nose. Cartilages are firm, but flexible tissues. There are many types of cartilages found in the body. Among them, articular cartilages are the ones that are present on the surface of the bones. As the name suggests articular cartilages exist to render articulation to the bones and retain t...more
Last Updated: 6 years ago• Featured Tip
Share
Bookmark
Report
Along with bones, the human structure is also supported by cartilage. Cartilage is a tough, flexible tissue that acts as a cushion between bones at joints. Some parts of the body such as the outer structure of the ear is completely made up of cartilage. Damage to the cartilage can cause pain, inflammation and in some cases even a degree of disability. Since cartilage does not have a blood supply, cartilage damage takes longer to heal than other injuries.
There are three main causes of c...more
There are three main causes of c...more
Last Updated: 6 years ago• Featured Tip
Share
Bookmark
Report
The shoulder is one of the most intricate joints in the body and given that it is subjected to a lot of lifting and movements, there are chances for it to tear or dislocate. The shoulder is a ball-and-socket joint with the socket in the shoulder, and the ball in the upper arm. The joint space between the two bones is surrounded by cartilage, and the space between the two is filled with fluid. Especially in athletes, due to forceful movement, this joint could get dislocated or the cartilage could...more
Last Updated: 6 years ago• Featured Tip
Share
Bookmark
Report
Skin is one of the most obvious parts of our body which ages with an increase in the number of candles on our birthday cakes. As you age, joints tend to become stiffer and less flexible. The body does not recover from bumps and bruises as easily as it did before, and it becomes difficult to stand for extended time intervals. This is caused mostly by a breakdown of cartilage and inflammation of the synovium.
What is cartilage?
Cartilage is a flexible connective tissue. It connects th...more
What is cartilage?
Cartilage is a flexible connective tissue. It connects th...more
Last Updated: 6 years ago• Featured Tip
Share
Bookmark
Report
Have you undergone cartilage damage recently and are seeking ideal treatment measures? Cartilage damage is a common form of injury that involves your knees. Other joints such as the ankles, elbows and hips may also be affected by cartilage damage. Cartilage, the tough and flexible tissues covering the surface of your joints, acts as a shock absorber, allowing the bones to slide over each other. Cartilage damage may occur because of injuries such as gradual wear, sports injuries and osteoarthriti...more
Last Updated: 6 years ago• Featured Tip
Share
Bookmark
Report
Cartilage is a tough, flexible tissue found throughout the body. It acts as a cushion between the bones and covers the surface of the joints. People having damaged cartilage often suffer from inflammation, stiffness and pain in joints.
What causes damage to the cartilage?
Direct blow: When the bones suffer from a direct blow during an accident or fall, the cartilage can get damaged. Athletes have a high risk of having damaged cartilage, particular those involved in wrestling, r...more
What causes damage to the cartilage?
Direct blow: When the bones suffer from a direct blow during an accident or fall, the cartilage can get damaged. Athletes have a high risk of having damaged cartilage, particular those involved in wrestling, r...more
Last Updated: 7 years ago• Featured Tip
Share
Bookmark
Report
Surgery for joint preservation is used to repair damaged articular cartilage because of osteoarthritis and malalignment. High Tibial Osteotomy is a medical or surgical method to realign the knee joint. This surgery especially helps people with knee arthritis to avoid knee replacement surgery, either partial or total, by maintaining injured joint tissues.
People suffering from degenerative arthritis or osteoarthritis encounter a high crushing of the articular cartilage and menisci that c...more
People suffering from degenerative arthritis or osteoarthritis encounter a high crushing of the articular cartilage and menisci that c...more
Last Updated: 7 years ago• Featured Tip
Share
Bookmark
Report
MBBS, Diploma In Orthopaedics, Trauma an...read more
Orthopedic Doctor•Visakhapatnam
Cartilage is a fine, rubbery elastic tissue that acts as cushion between the bones in the joint spaces. It is a connective tissue and enables the joints to move freely and smoothly. It acts as a shock absorber and reduces the friction between the joints. This cartilage could either be damaged as a result of injury or degeneration as part of normal ageing process. Either of this causes friction during joint movement, causing painful, stiff movements and in some cases, even swelling of the joint s...more
Last Updated: 7 years ago• Featured Tip
Share
Bookmark
Report
When it comes to contact sports like football or basketball, orthopaedic injuries are unavoidable. Given the high risk of falling and accidents and wear and tear of muscles, injuries like stress fractures, torn ligaments, ACL tears and chronic pain are common complaints a sports doctor comes across. Sports medicine is a specialisation of this field that deals exclusively with the prevention, diagnosis and treatment of injuries sustained while playing sports. A sports doctor must not only treat a...more
Last Updated: 7 years ago• Featured Tip
Share
Bookmark
Report
Cartilage is an important structural component of human body. It is found in various parts of body like joints, end of ribs, nose, ears, and airway tube.
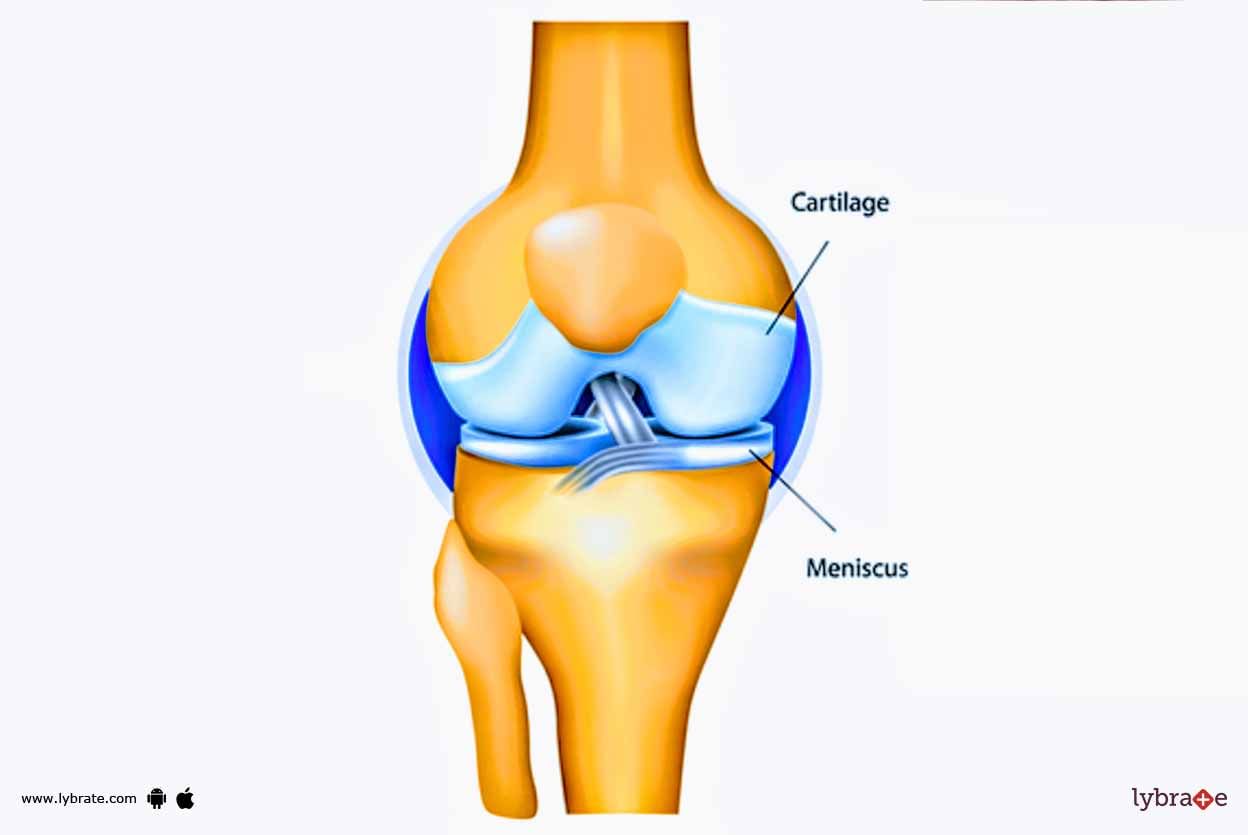
Knee joint contains 2 types of cartilage. 1st is the type which lines the surface of bones. 2nd type lies between the two joint forming bones and is called Meniscus. This article is about 1st type which is also called as articular cartilage.
Articular cartilage works as a lubricated surface and reduces joint friction. It plays...more
Knee joint contains 2 types of cartilage. 1st is the type which lines the surface of bones. 2nd type lies between the two joint forming bones and is called Meniscus. This article is about 1st type which is also called as articular cartilage.
Articular cartilage works as a lubricated surface and reduces joint friction. It plays...more
Book appointment with top doctors for Cartilage Surgery treatment
View fees, clinic timings and reviews
Ask a free question
Get FREE multiple opinions from Doctors
posted anonymously