Get the App
For Doctors
Login/Sign-up
About
Health Feed
Find Doctors
Health Packages
AllQ&AsTipsQuizzes
Blister Tips
Last Updated: 3 years ago• Featured Tip
Share
Bookmark
Report
Boil, also known as a skin abscess, is a painful and unsightly condition that affects people of all ages. It is caused by a bacterial infection in a hair follicle or oil gland, leading to the formation of a painful, red bump filled with pus. Boils can be especially debilitating, as they can cause intense pain and discomfort, making it difficult to carry out everyday activities.
;
People with weakened immune systems, poor hygiene, and those who live in crowd...more
Last Updated: 3 years ago• Featured Tip
Share
Bookmark
Report
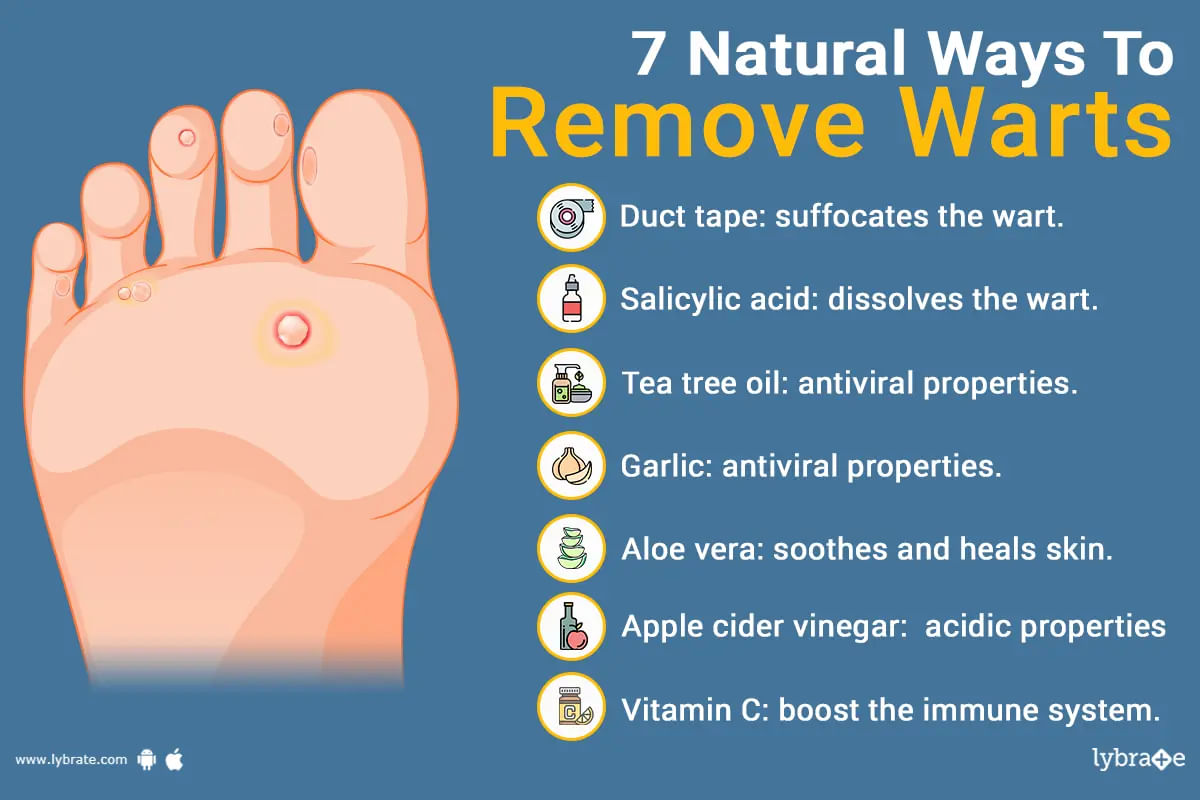
There is a virus, human papillomavirus (hpv), that infect humans which causes a type of skin infection called warts. This infection to skin causes it to form skin-color bumps which may be hard and rough. This infection can be transferred by touching the person who has it because it is contagious. Feet, hands, thigh, genitals, neck are the places of occurrence of these warts. These warts are non cancerous but grow like cancerous mass of skin. A cut or break in skin can be the ...more
Last Updated: 6 years ago• Featured Tip
Share
Bookmark
Report
Pityriasis lichenoides is referred to a rare type of rash which is characterized by tiny papules that voluntarily flatten and relapse within a period of weeks. This condition which can range from moderate to severe in nature can be either chronic or acute. In the severest cases, it may develop into reddish-brown blisters and crusts.
Causes and Symptoms
This condition which is chiefly prevalent in teenagers and adults is slightly likelier to appear in males. This condition is ex...more
Causes and Symptoms
This condition which is chiefly prevalent in teenagers and adults is slightly likelier to appear in males. This condition is ex...more
Last Updated: 6 years ago• Featured Tip
Share
Bookmark
Report
What are Cold Sores?
Cold sores are also called as fever blisters. Fever blisters are a common viral infection. Cold sores are red, fluid-filled blisters that form near the mouth or on other areas of the face. These blisters are often grouped together in patches. Cold sores usually heal in two to four weeks without leaving a scar.
Risk factors -
Infection, fever, or a cold
Stress
Sun exposure and severe burns
Cancer chemotherapy
Menstruation and eczema
H...more
Cold sores are also called as fever blisters. Fever blisters are a common viral infection. Cold sores are red, fluid-filled blisters that form near the mouth or on other areas of the face. These blisters are often grouped together in patches. Cold sores usually heal in two to four weeks without leaving a scar.
Risk factors -
Infection, fever, or a cold
Stress
Sun exposure and severe burns
Cancer chemotherapy
Menstruation and eczema
H...more
Last Updated: 6 years ago• Featured Tip
Share
Bookmark
Report
Are you observing bumps and lesions in and around your vagina? These are female genital sores, which may be painful, itchy, produce a discharge, and are very tender. These lumps and sores may occur due to skin disorders. Female genital sores mostly appear as a symptom of STIs or sexually transmitted infections. STIs are considered to be a hidden epidemic, which many women leave untreated because of embarrassment or fear.
Diagnosis of female genital sores
A physical examination is co...more
Diagnosis of female genital sores
A physical examination is co...more
Last Updated: 6 years ago• Featured Tip
Share
Bookmark
Report
What is pemphigus Vulgaris?
Pemphigus Vulgaris is a rare autoimmune disorder of the skin which produces blisters and sores of the skin and mucous membranes. Depending on the appearance of blisters it can be of two types:
Pemphigus Vulgaris: painful blisters appear in the mouth in the beginning and then spread to genitals and skin. They are more sore and painful but don t itch.
Pemphigus foliaceus: blisters appear on the chest, back and shoulders which itch more and are less pain...more
Pemphigus Vulgaris is a rare autoimmune disorder of the skin which produces blisters and sores of the skin and mucous membranes. Depending on the appearance of blisters it can be of two types:
Pemphigus Vulgaris: painful blisters appear in the mouth in the beginning and then spread to genitals and skin. They are more sore and painful but don t itch.
Pemphigus foliaceus: blisters appear on the chest, back and shoulders which itch more and are less pain...more
Last Updated: 6 years ago• Featured Tip
Share
Bookmark
Report
Diabetes can be a life-threatening condition if you do not keep blood glucose levels in control. Suffering from diabetes for a prolonged period can lead to a number of associated diseases in different parts of the body. Diabetic foot is one such condition that diabetes patients suffer from in some instances.
What is diabetic foot?
Diabetes causes degeneration of the nerves in the legs. This is known as diabetic neuropathy, which is a type of diabetic foot. If diabetes adversely...more
What is diabetic foot?
Diabetes causes degeneration of the nerves in the legs. This is known as diabetic neuropathy, which is a type of diabetic foot. If diabetes adversely...more
Last Updated: 7 years ago• Featured Tip
Share
Bookmark
Report
हमारे बॉडी की ऊपरी त्वचा के परत पर फफोले यानी ब्लिस्टर हो जाते हैं. अलग-अलग लोगों में अलग-अलग तरीके से होते हैं. इनमें जलन, लगातार घर्षण से इन्फेक्शन भी हो जाते हैं. इनके लिए कई घरेलू उपचार हैं. त्वचा की ऊपरी परत पर कई कारणों से फफोले पड़ जाते हैं. त्वचा के जलने, जमने, उस पर कुछ रगड़ लग जाने या फिर किसी इन्फेक्शन की वजह से होने वाले इन फफोलों में पानी जैसा कोई द्रव भी भरा होता है और आमतौर पर ये फूले हुए लगते हैं. इसमें भरा द्रव सीरम या प्लाज्मा कहलाता है. इसके अलावा कुछ अन्य मामलों में इन फफोलों...more
Last Updated: 7 years ago• Featured Tip
Share
Bookmark
Report
Diabetes is a deadly disease that is triggered when the body cannot produce enough insulin or becomes resistant to insulin. Diabetes makes an individual prone to a host of ailments, one of which is a diabetic foot.
What is diabetic foot?
When blood sugar remains high for protracted periods, it affects the feet in a number of ways and leads to a condition called a diabetic foot. There are two types of diabetic foot-
Diabetic neuropathy: Diabetes dulls or even damages ...more
What is diabetic foot?
When blood sugar remains high for protracted periods, it affects the feet in a number of ways and leads to a condition called a diabetic foot. There are two types of diabetic foot-
Diabetic neuropathy: Diabetes dulls or even damages ...more
Last Updated: 7 years ago• Featured Tip
Share
Bookmark
Report
Collectively grouped under the Ewing sarcoma family of tumors, Ewing's sarcoma is the second most common primary bone cancer occurring predominantly in children and in adolescents. Very rarely is it experienced in adults above the age of 30.
Typically forming in the bones of the chest, pelvis, head, back or trunk and in the long bones of the arms and legs, Ewing's sarcoma is believed to originate in certain kinds of primitive cells. When it begins to affect similar kind of cells found o...more
Typically forming in the bones of the chest, pelvis, head, back or trunk and in the long bones of the arms and legs, Ewing's sarcoma is believed to originate in certain kinds of primitive cells. When it begins to affect similar kind of cells found o...more
Book appointment with top doctors for Blister treatment
View fees, clinic timings and reviews
Ask a free question
Get FREE multiple opinions from Doctors
posted anonymously