Diabetes & Oral Heath Problems!
People with diabetes are at higher risk for oral health problems, such as gingivitis (an early stage of gum disease) and periodontitis (serious gum disease) because they are generally more susceptible to bacterial infection, and have a decreased ability to fight bacteria that invade the gums.
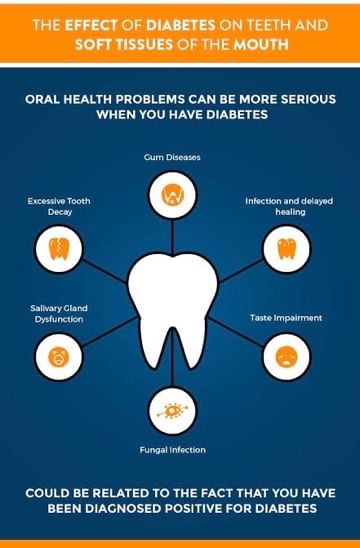
If diabetes is left untreated, it can cause following symptoms in the mouth:
- you may have less saliva, causing your mouth to feel dry. (dry mouth is also caused by certain medications). Drymouth can cause soreness, ulcers, infections and cavities.
- gums may become inflamed and bleed often (gingivitis).
- you may have problems tasting food.
- you may experience delayed wound healing.
- you may be susceptible to infections inside of your mouth.
- other oral problems associated with diabetes include thrush, an infection caused by the fungus that grows in the mouth.
There is a two-way street!- emerging research also suggests that the relationship between serious gum disease and diabetes is two-way. Not only are people with diabetes more susceptible to serious gum disease, but serious gum disease may have the potential to affect blood glucose control and contribute to the progression of diabetes.
Your diabetes dental health action plan-
Self-care and professional care at the dental clinic will be beneficial in keeping your healthy smile as well as potentially slowing the progression of diabetes. Here are five oral health-related things you can do to for optimal wellness:
- control your blood sugar levels. Use your diabetes-related medications as directed, changing to a healthier diet and even exercising more can help. Good blood sugar control will also help your body fight any bacterial or fungal infections in your mouth and help relieve dry mouth caused by diabetes.
- avoid smoking.
- if you wear any type of denture, clean it each day.
- make sure to brush twice a day with and clean between your teeth daily.
- keep your dental visits regular


+1.svg)
